Skin mycoses are a large group of fungal diseases caused by dermatophytes – filamentous fungi from the genera Epidermophyton, Trichophyton, Microsporum, etc. These fungi are widespread in nature, have a pronounced contagiousness and can be divided into:
- Geophilic – transmitted by direct contact with soil, affect people sporadically, usually spread by spores that can live for years;
- Zoophilic – transmitted from animals through direct contact, or indirect – through objects on which there is contaminated animal hair;
- Anthropophilic – transmitted from person to person through direct contact or through household items.
There are the following types of mycosis of the skin: tinea corporis (mycosis of the trunk), tinea manus (mycosis of the hands), tinea pedis (mycosis of the feet), tinea cruris (mycosis of the groin area).
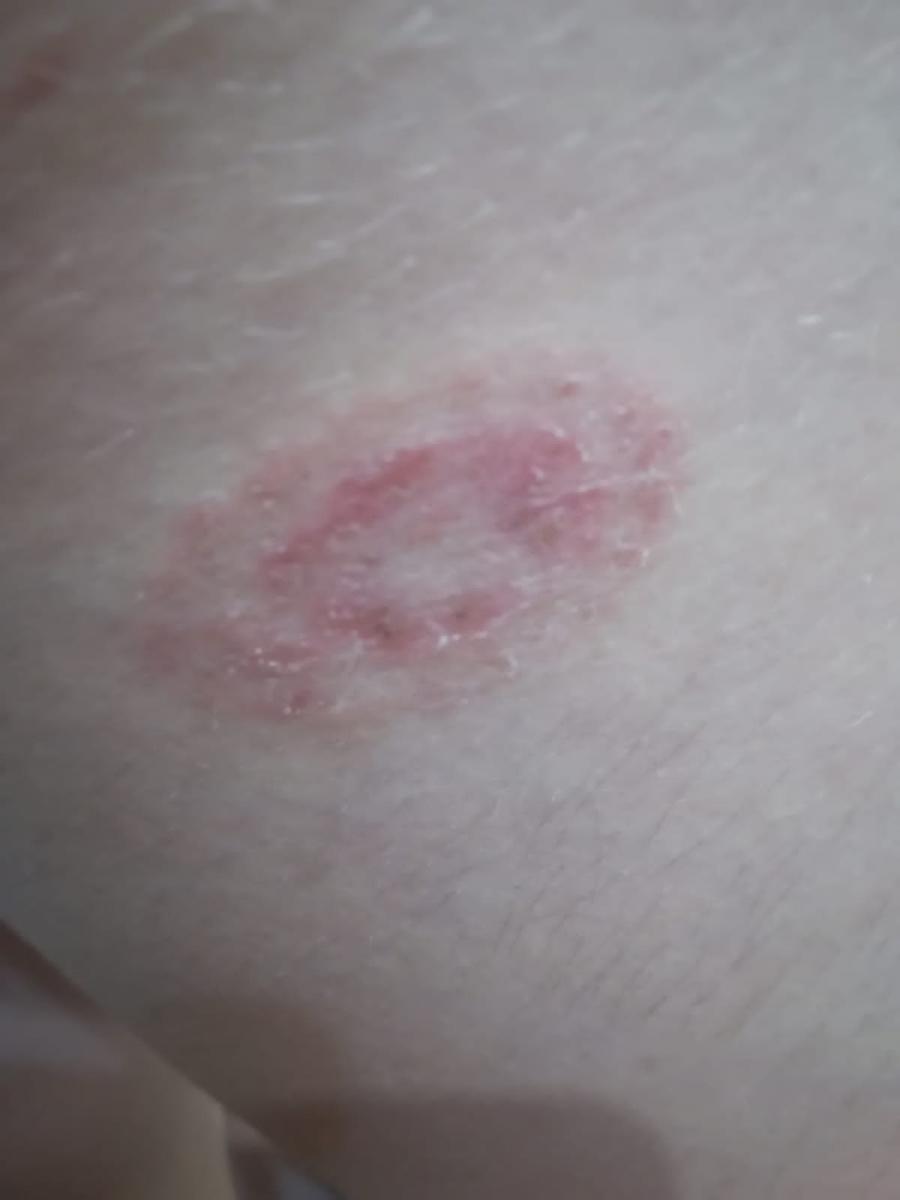
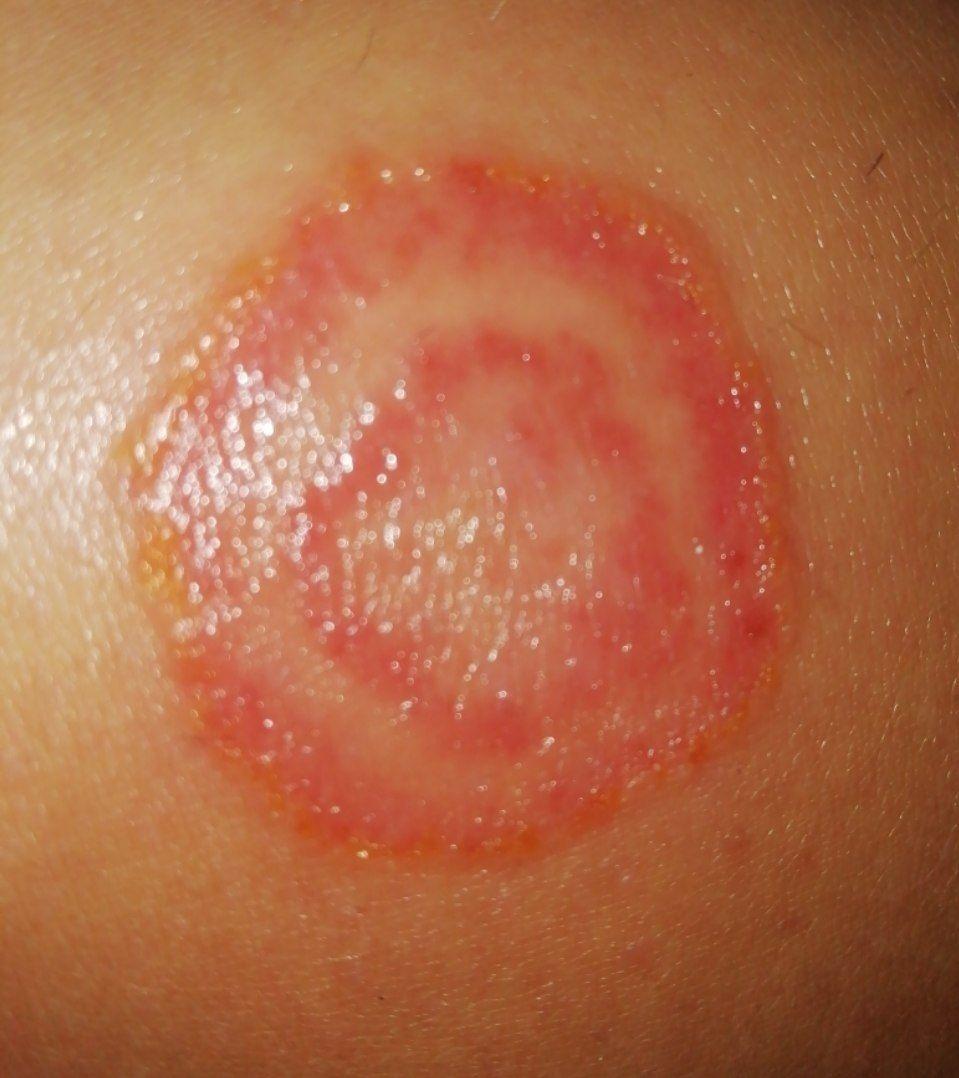
Tinea corporis
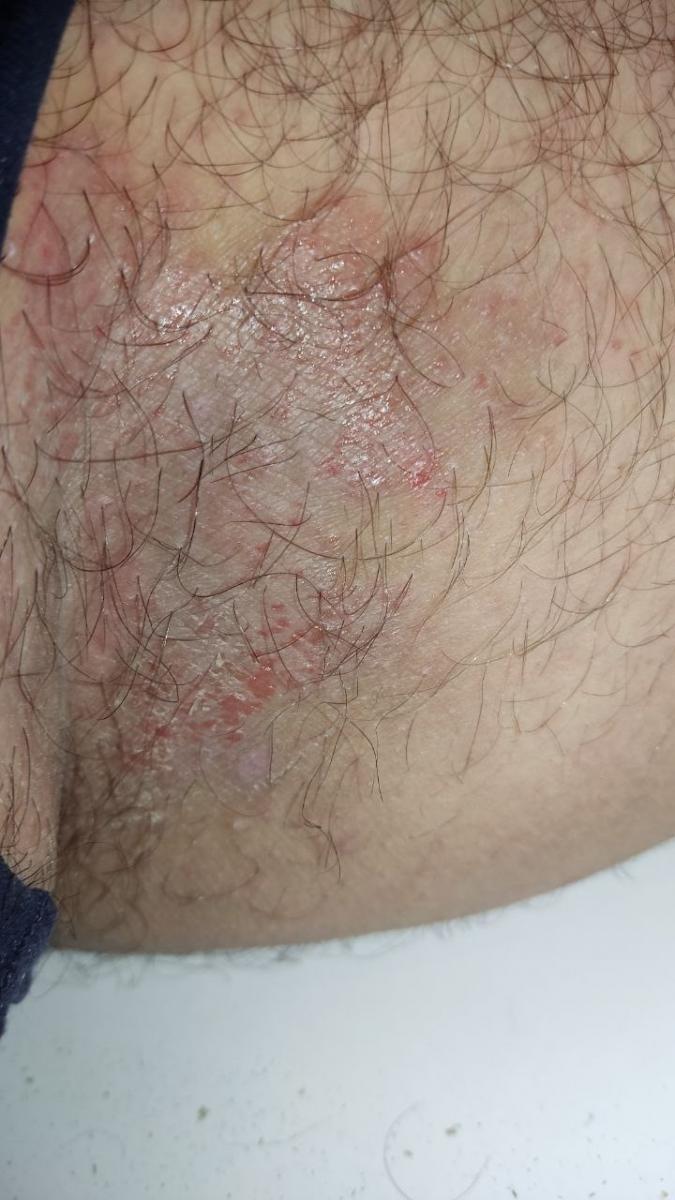
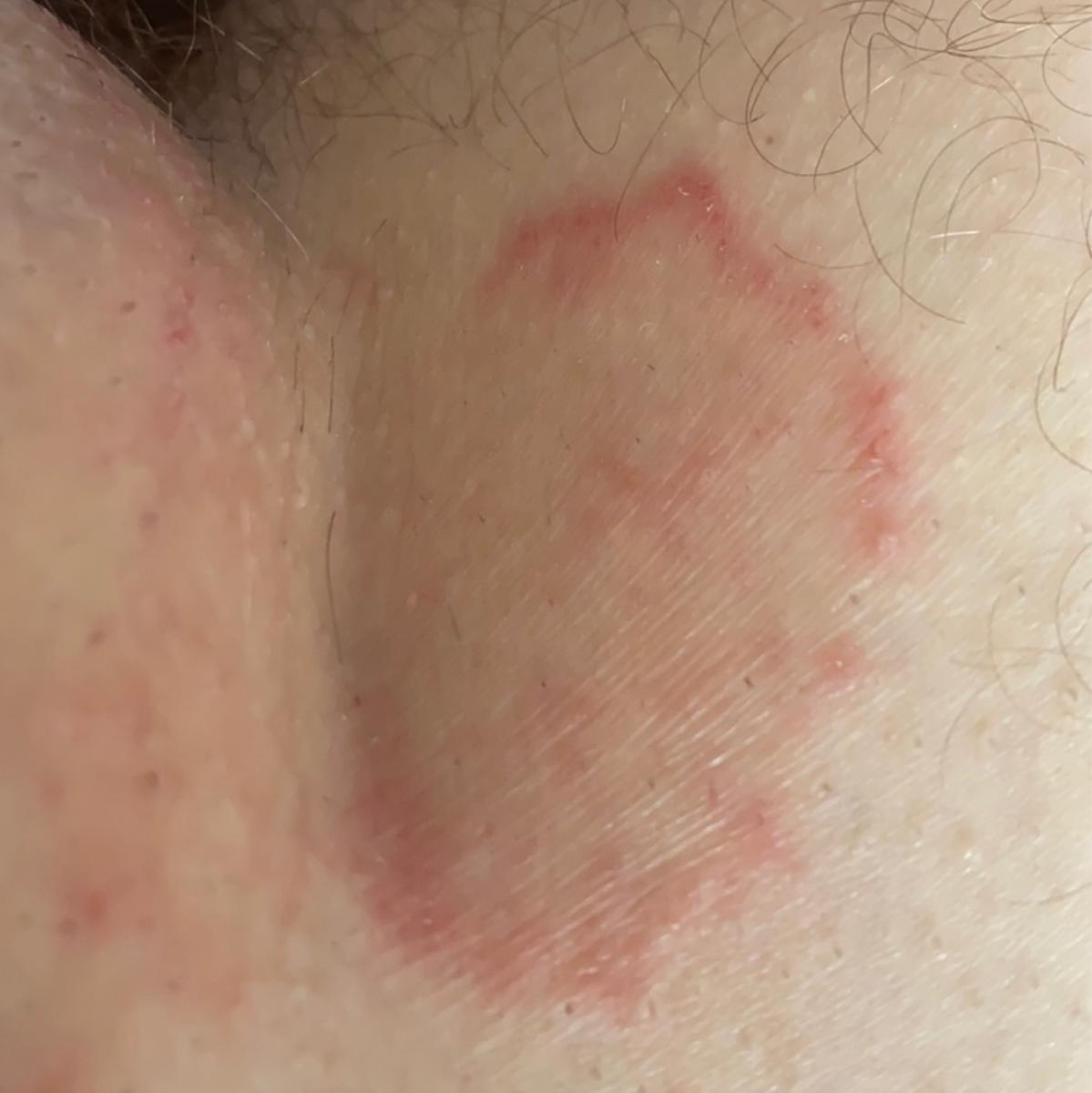
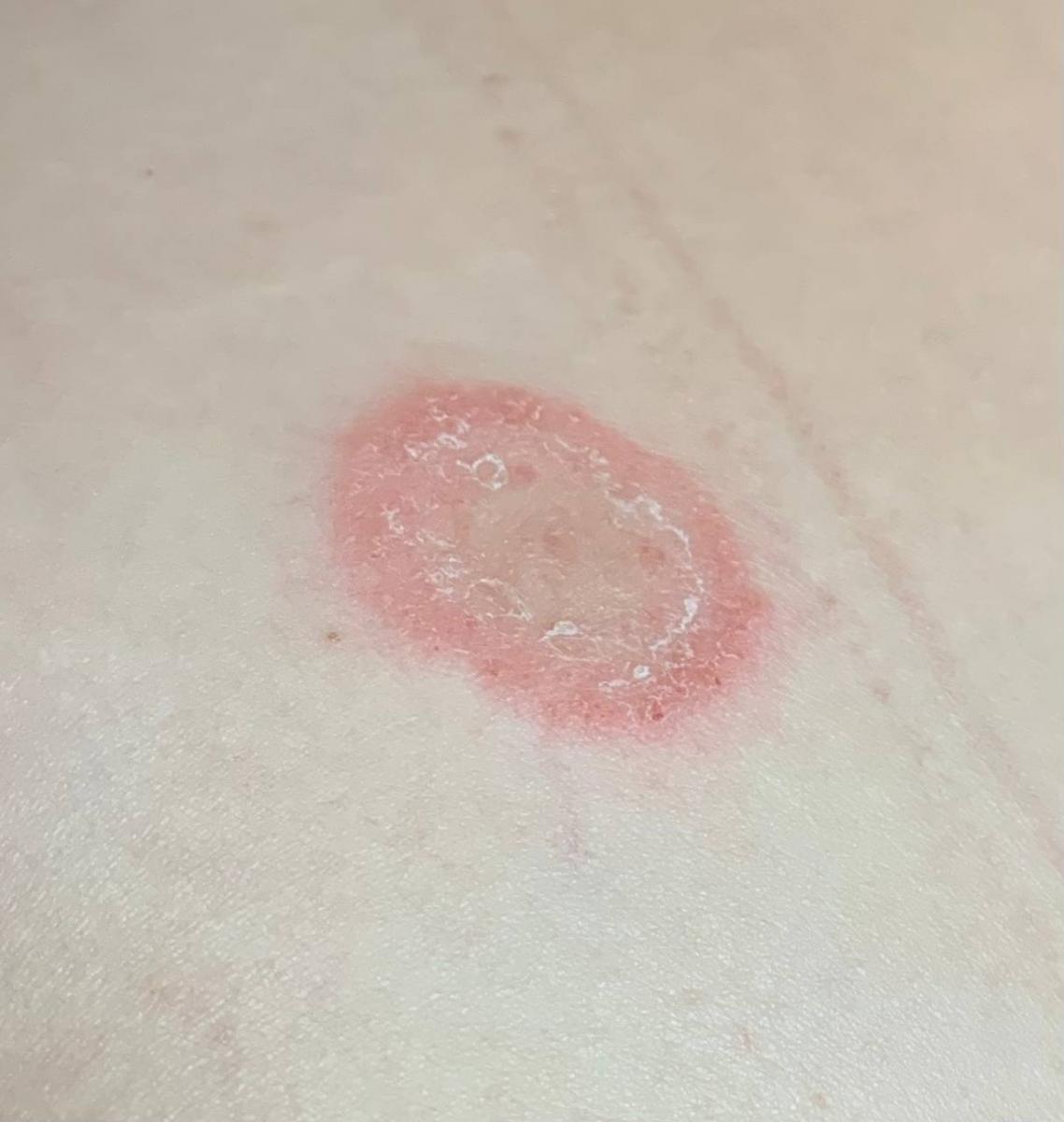
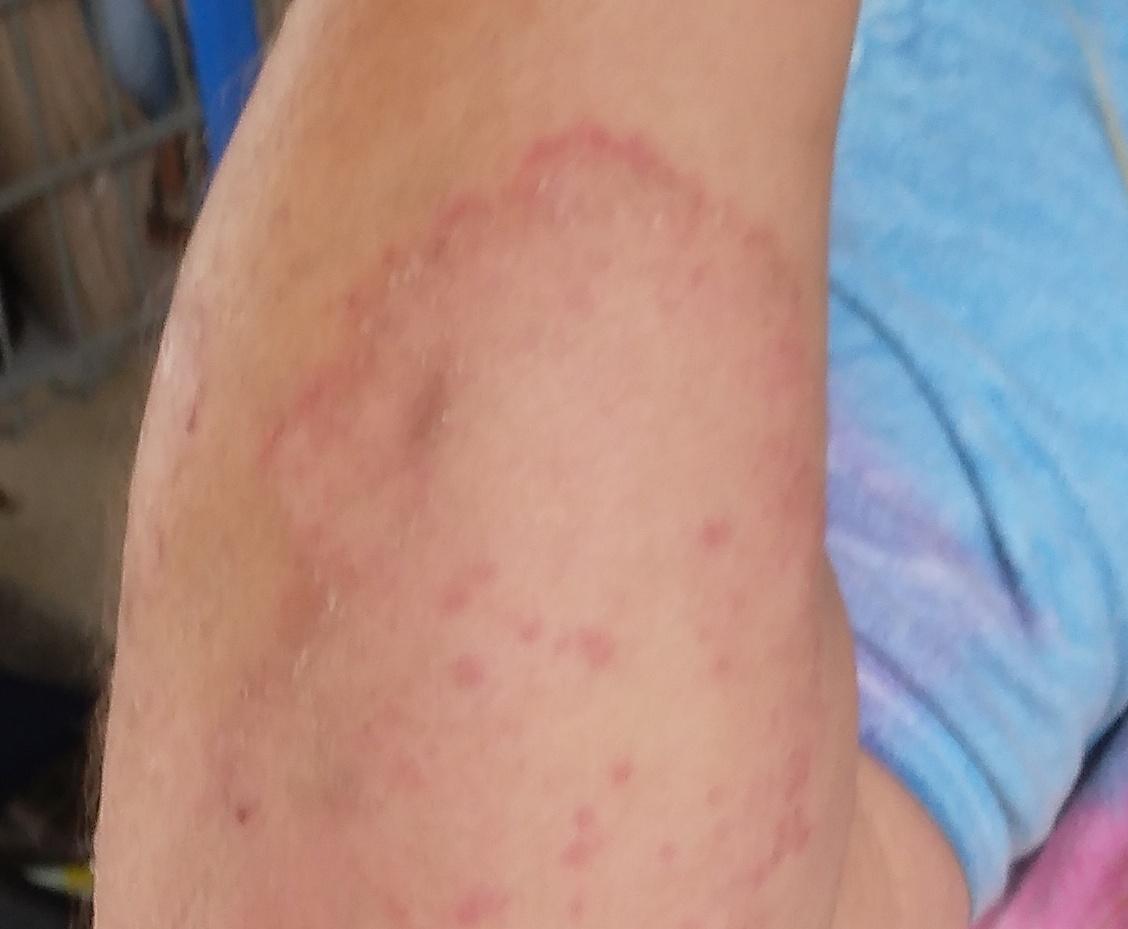
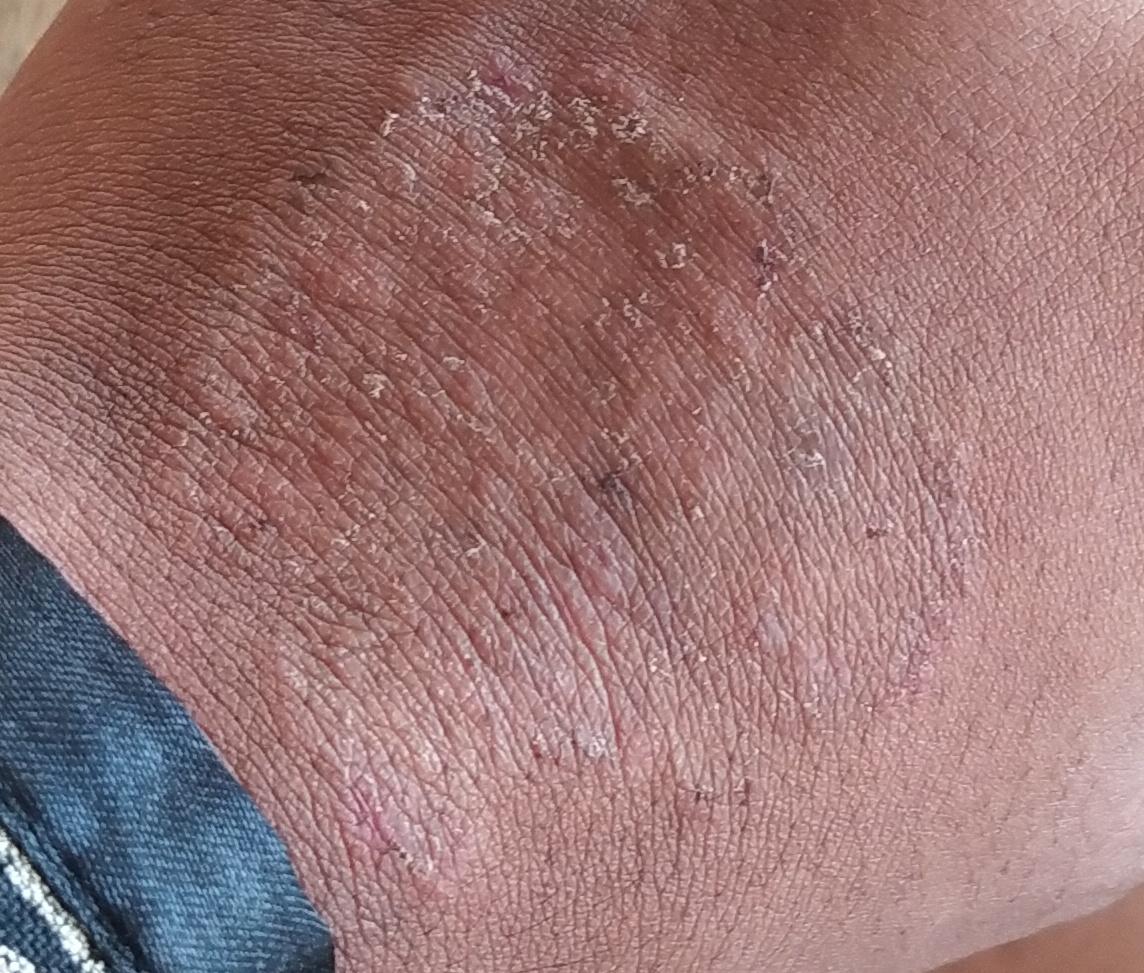
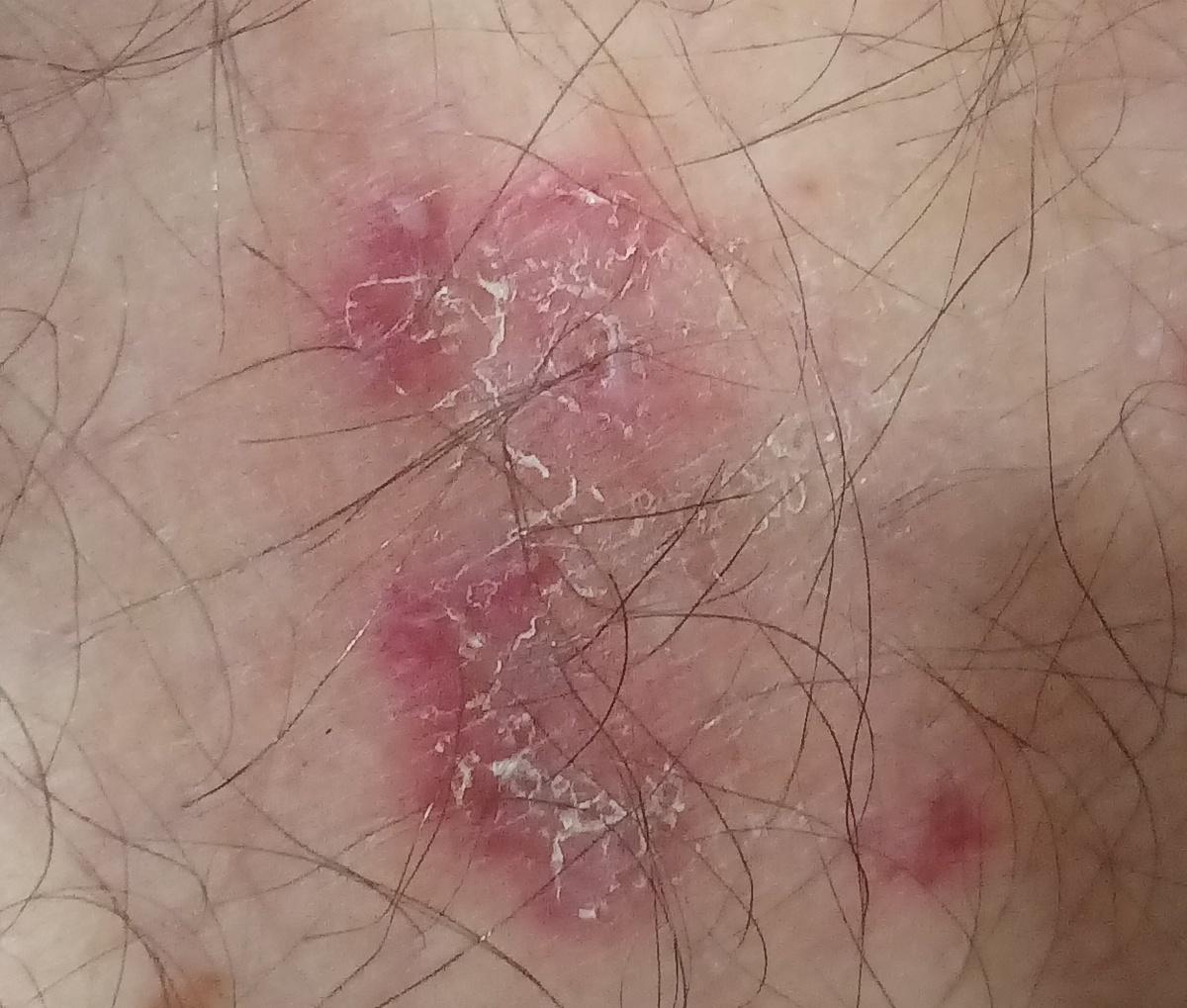
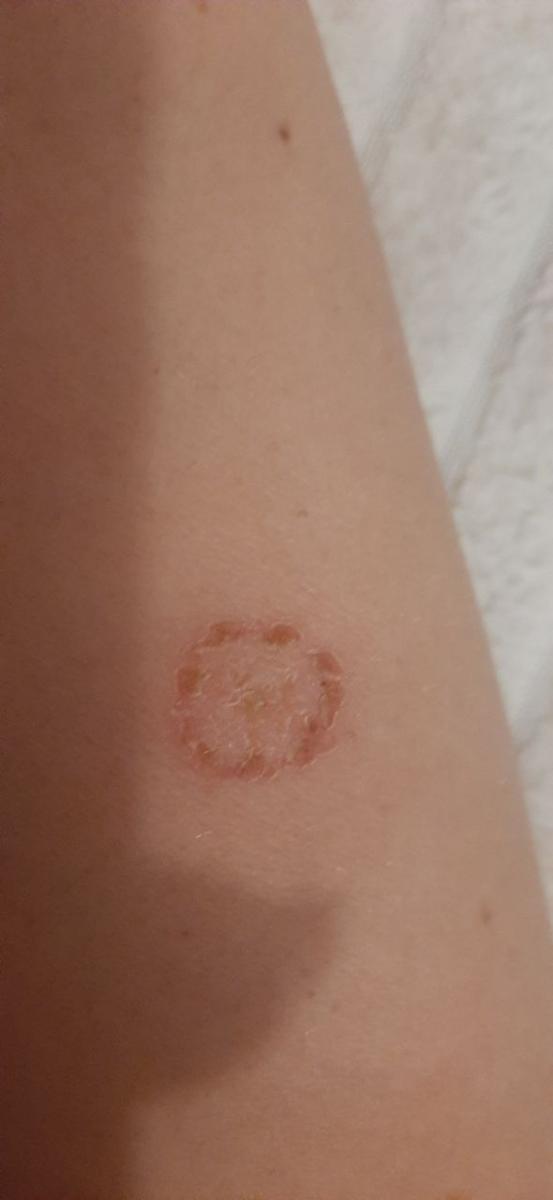
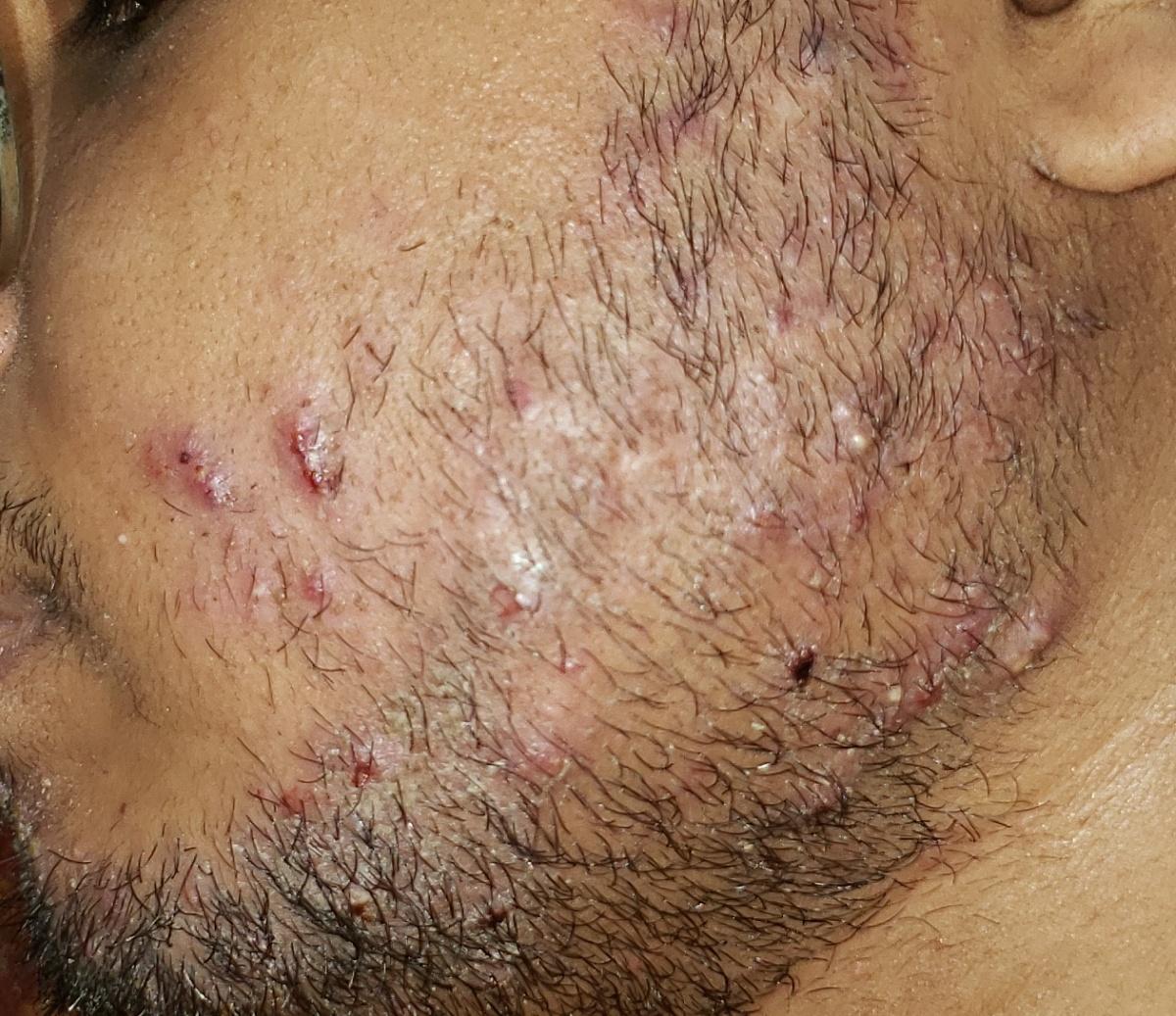
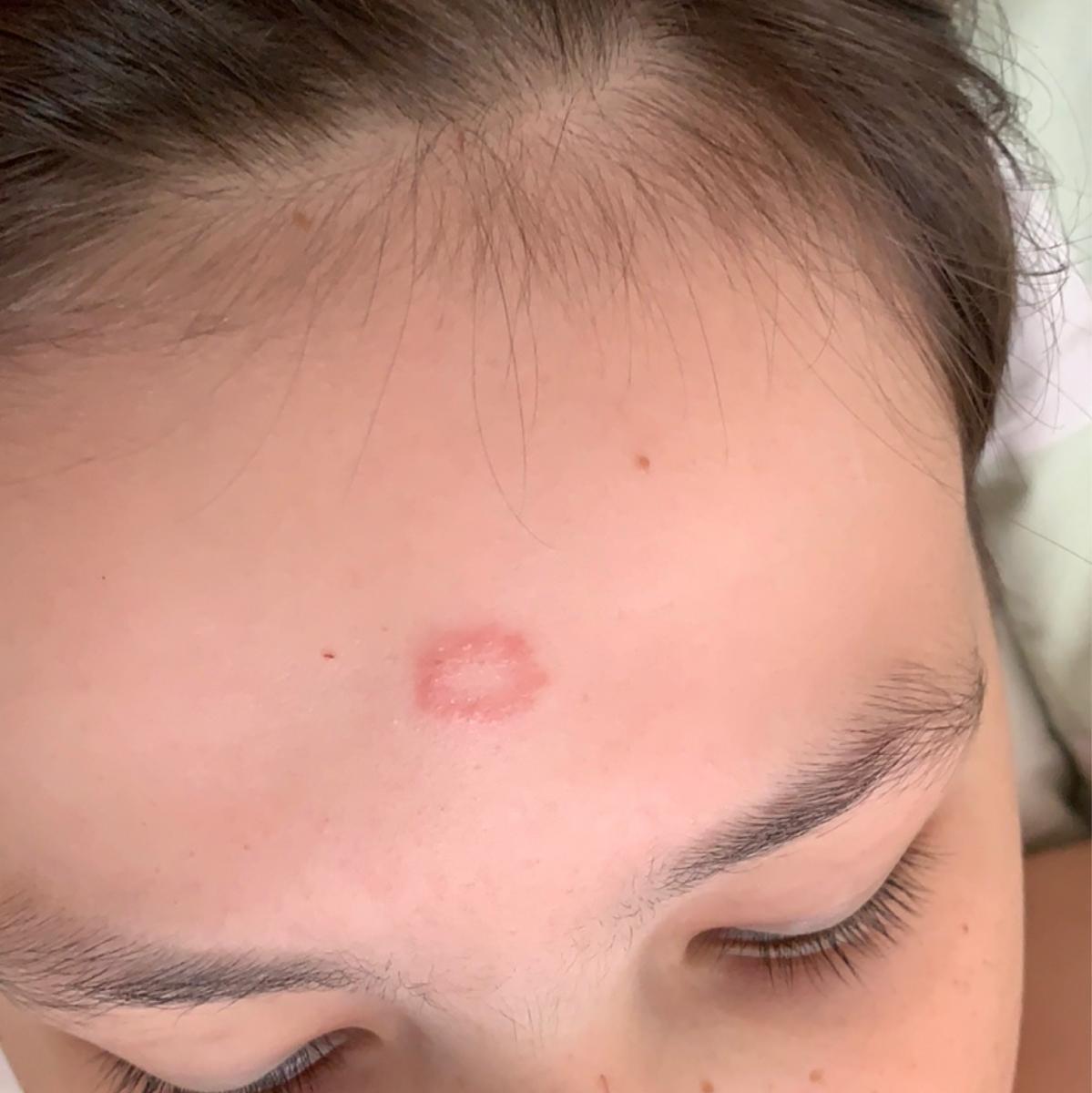
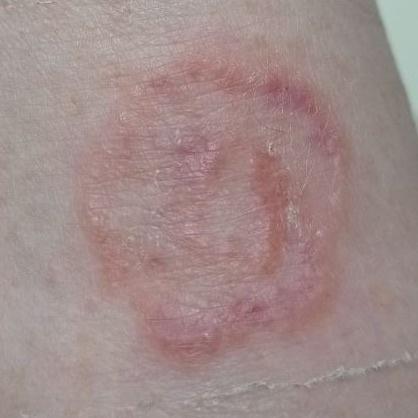
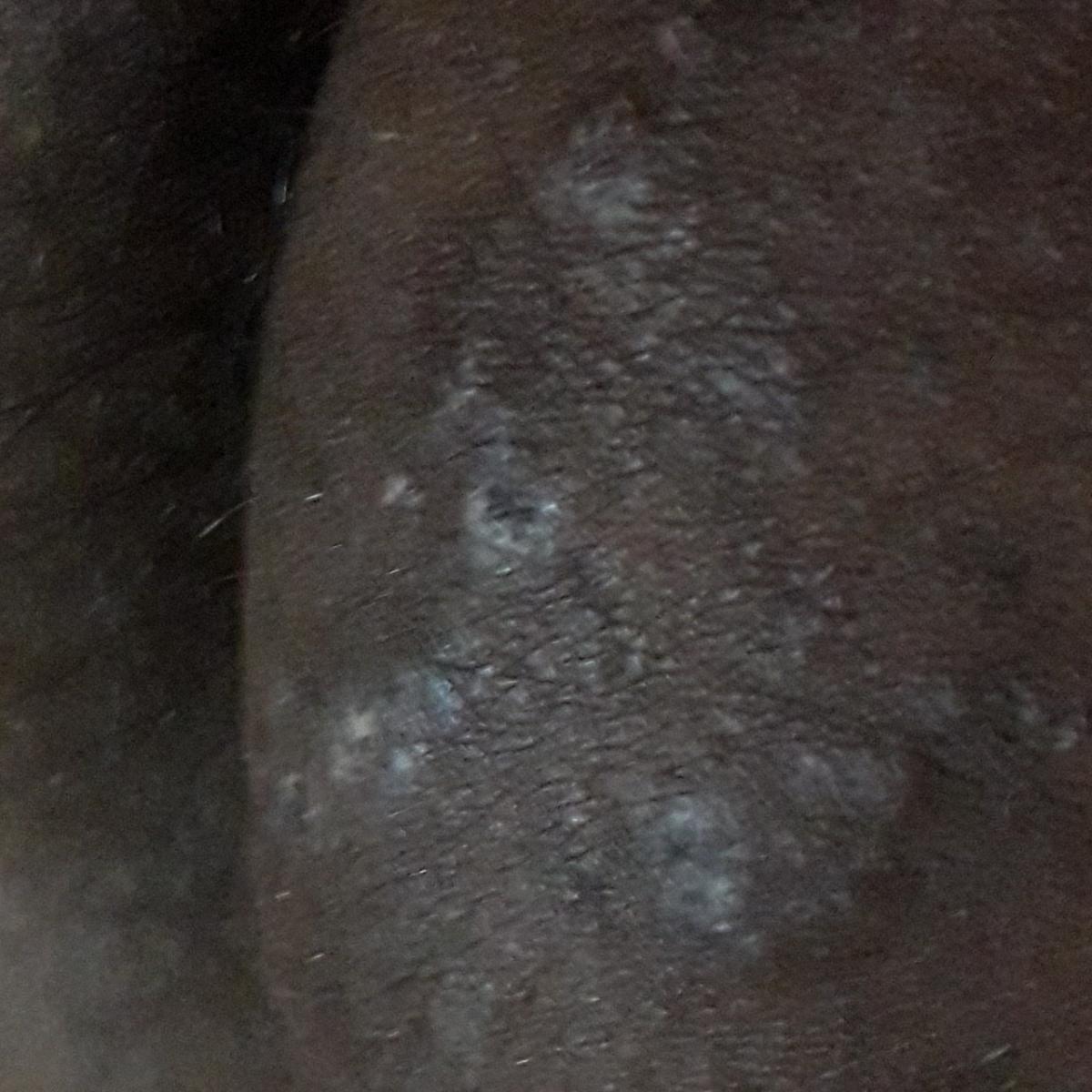
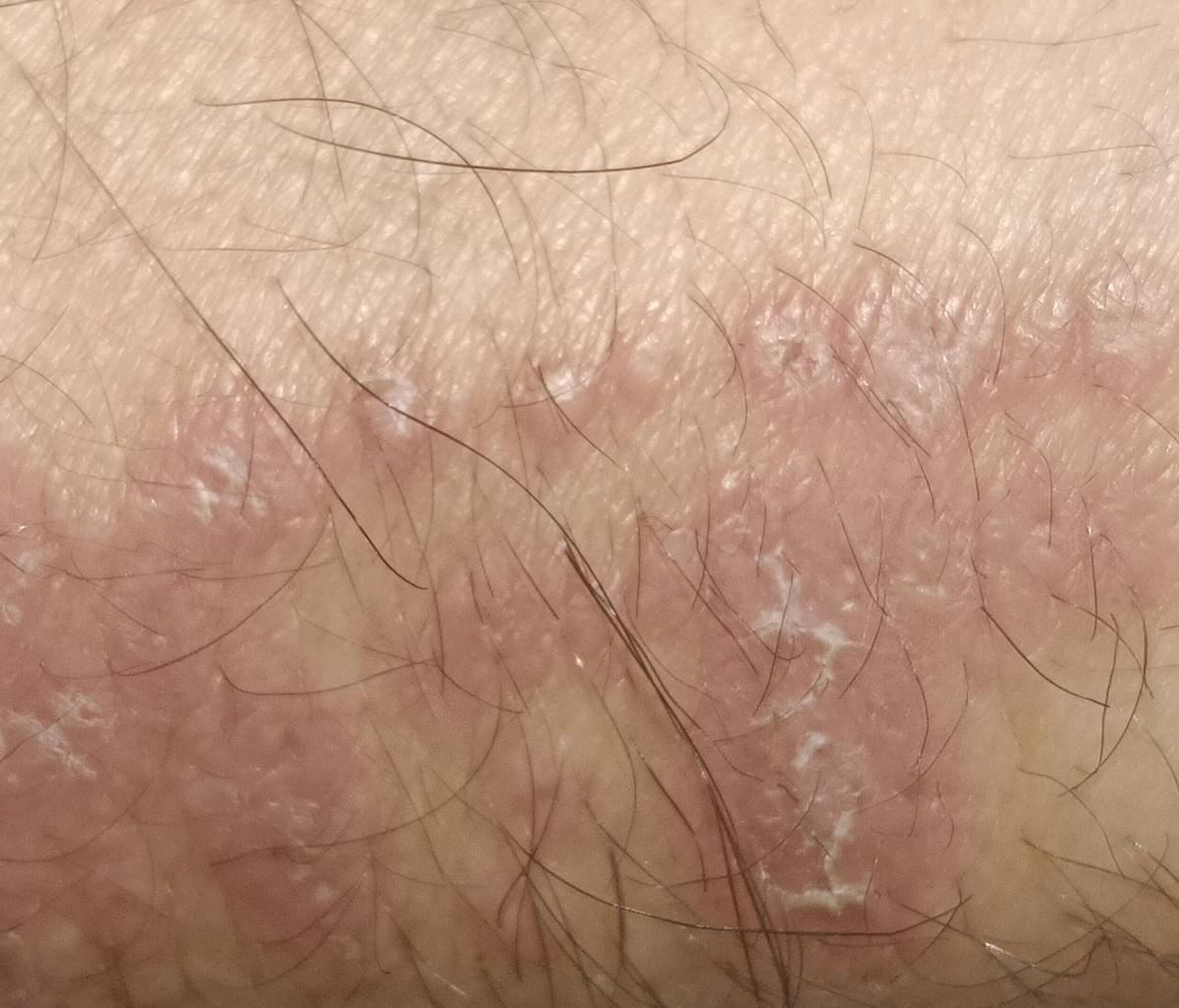
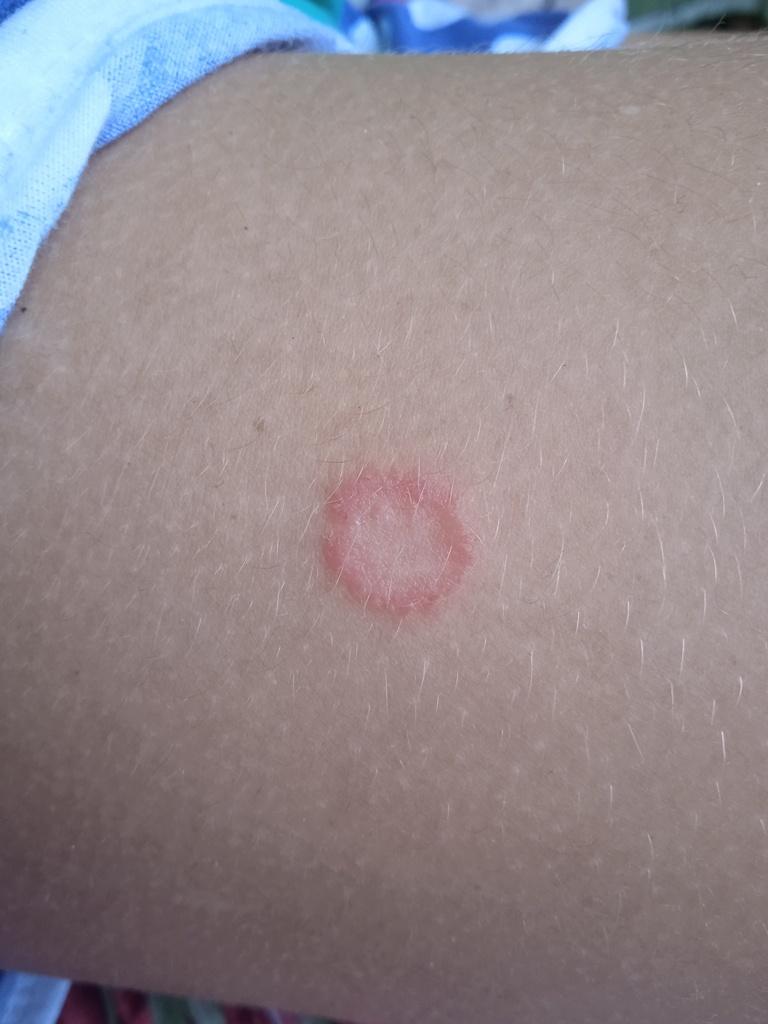
Smooth skin mycoses include all skin mycoses of the trunk and extremities, with the exception of hair, nails, palms, soles and folds. It can appear on any part of the body. More common in tropical regions. Any dermatophyte can potentially cause smooth skin dermatophytosis, but the most common pathogens are Microsporum canis (zoophilic) and Tr. rubrum (anthropophilic).
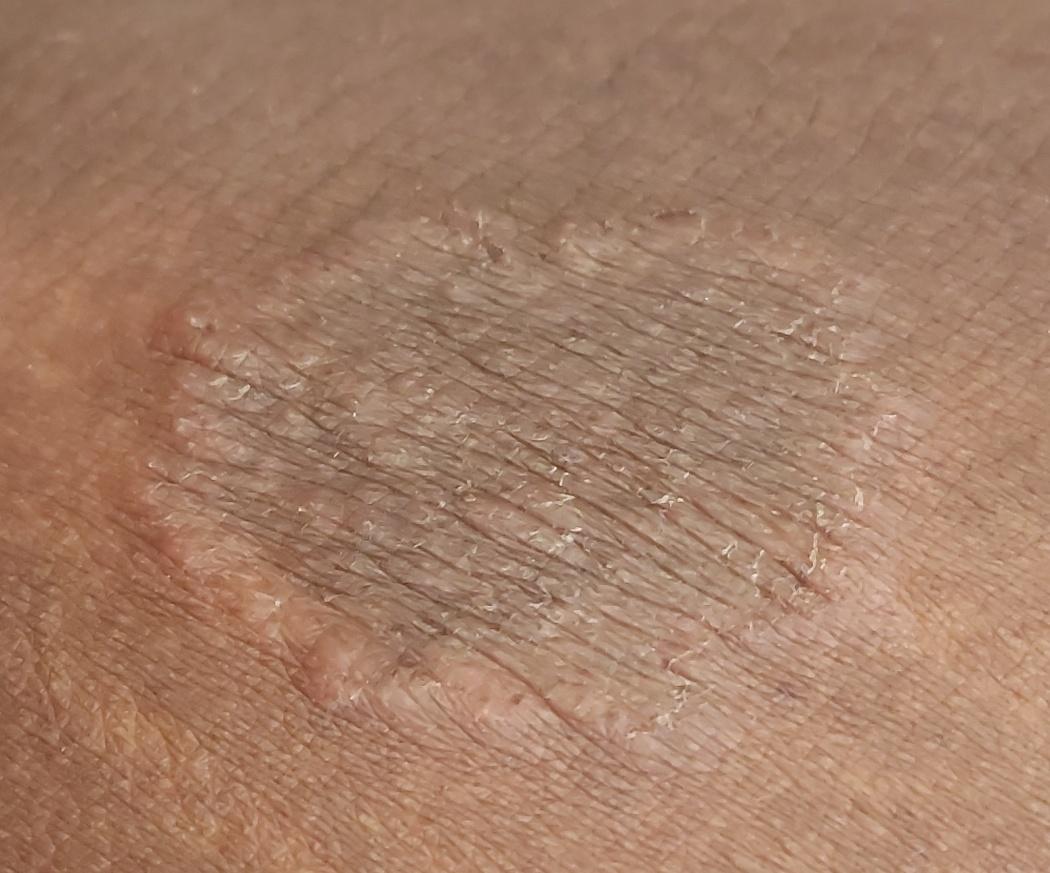
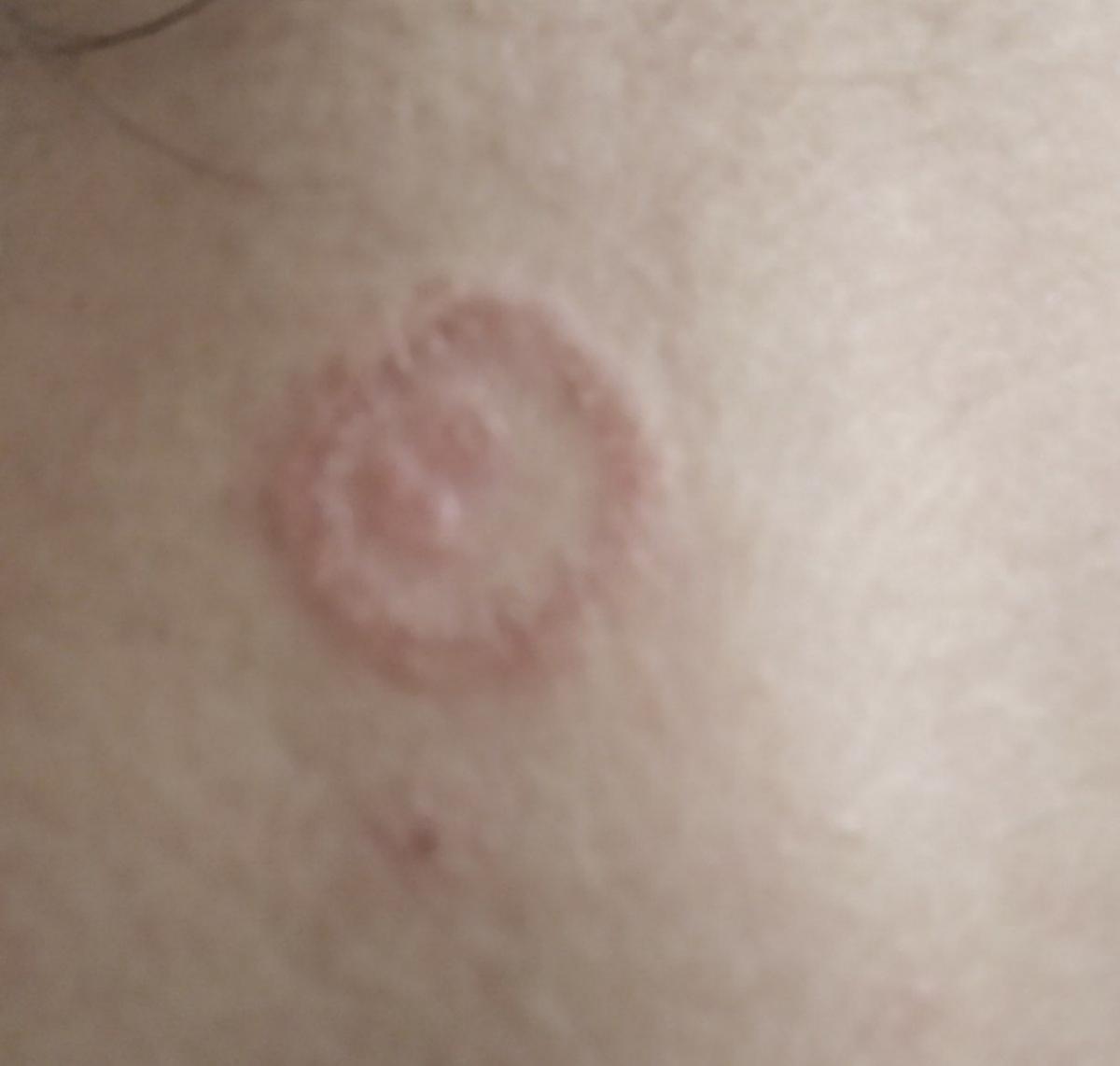
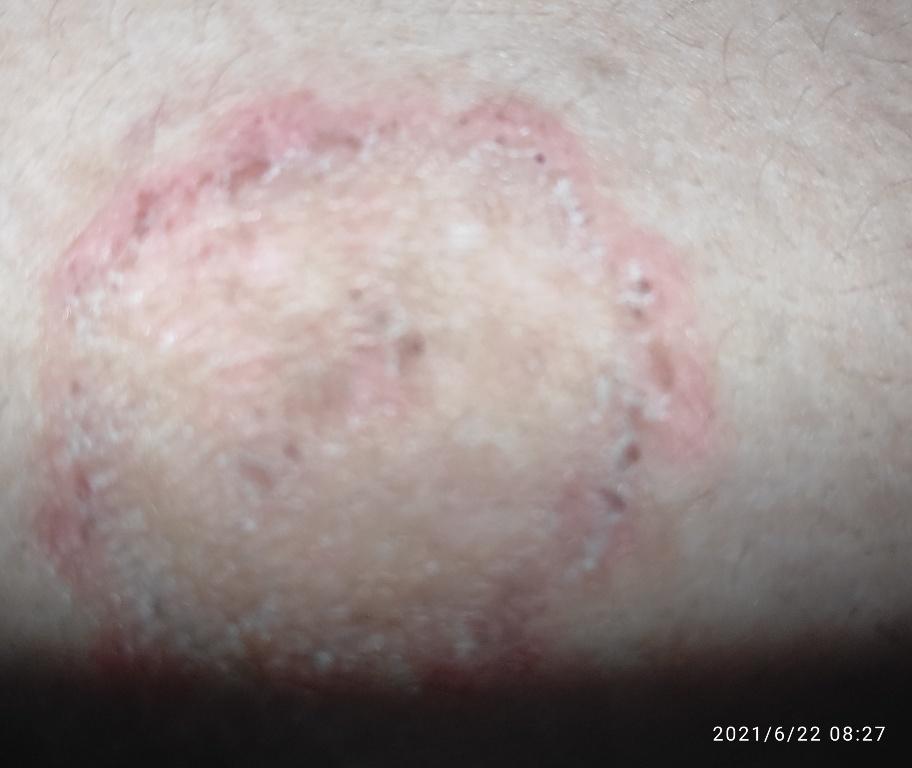
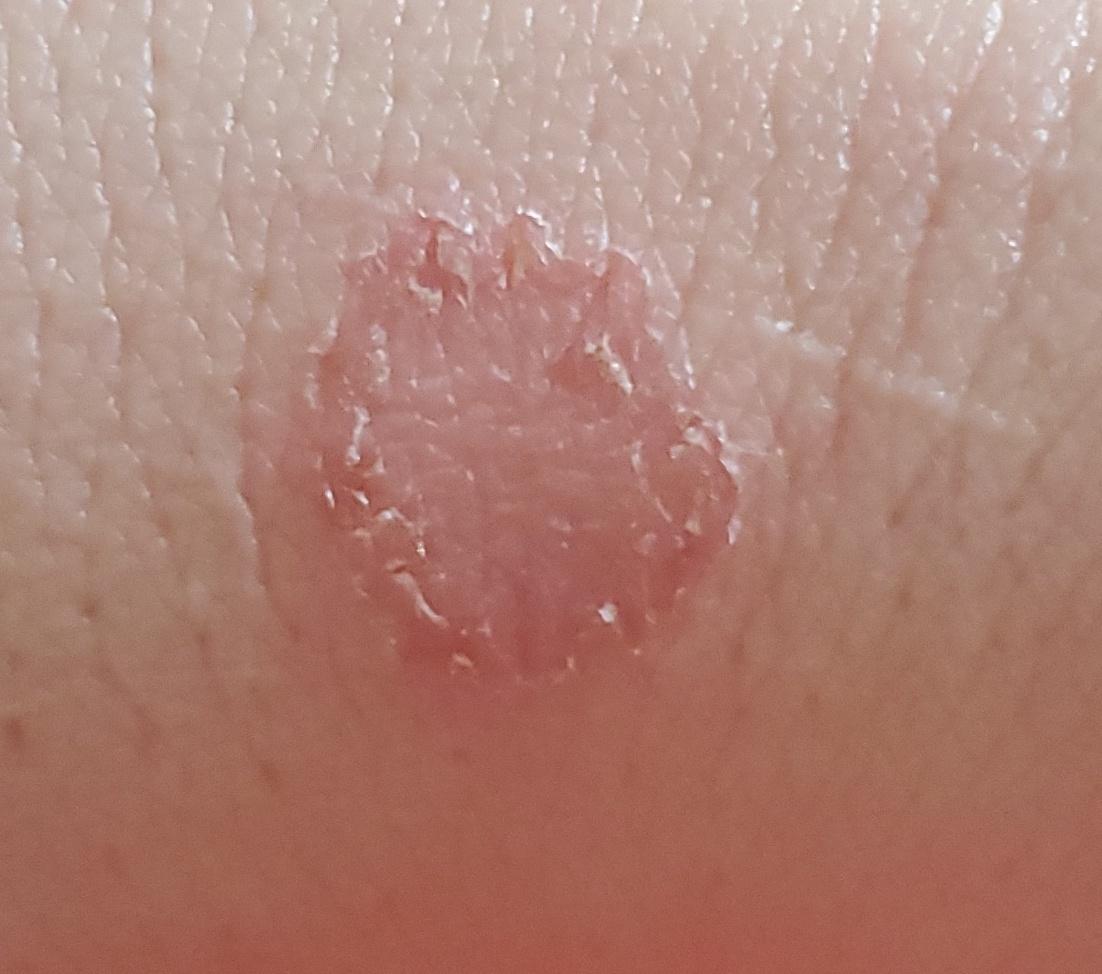
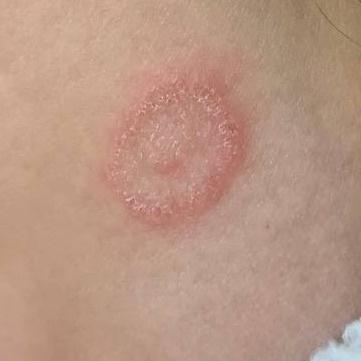
The clinical picture is presented by many variants of mycosis of smooth skin. The classic manifestations are ring-shaped eruptions with scales along the entire erythematous border. The border is usually vesicular and thickens towards the center. The center of the rash is usually scaly. The rash can be “creeping” and ring-shaped.
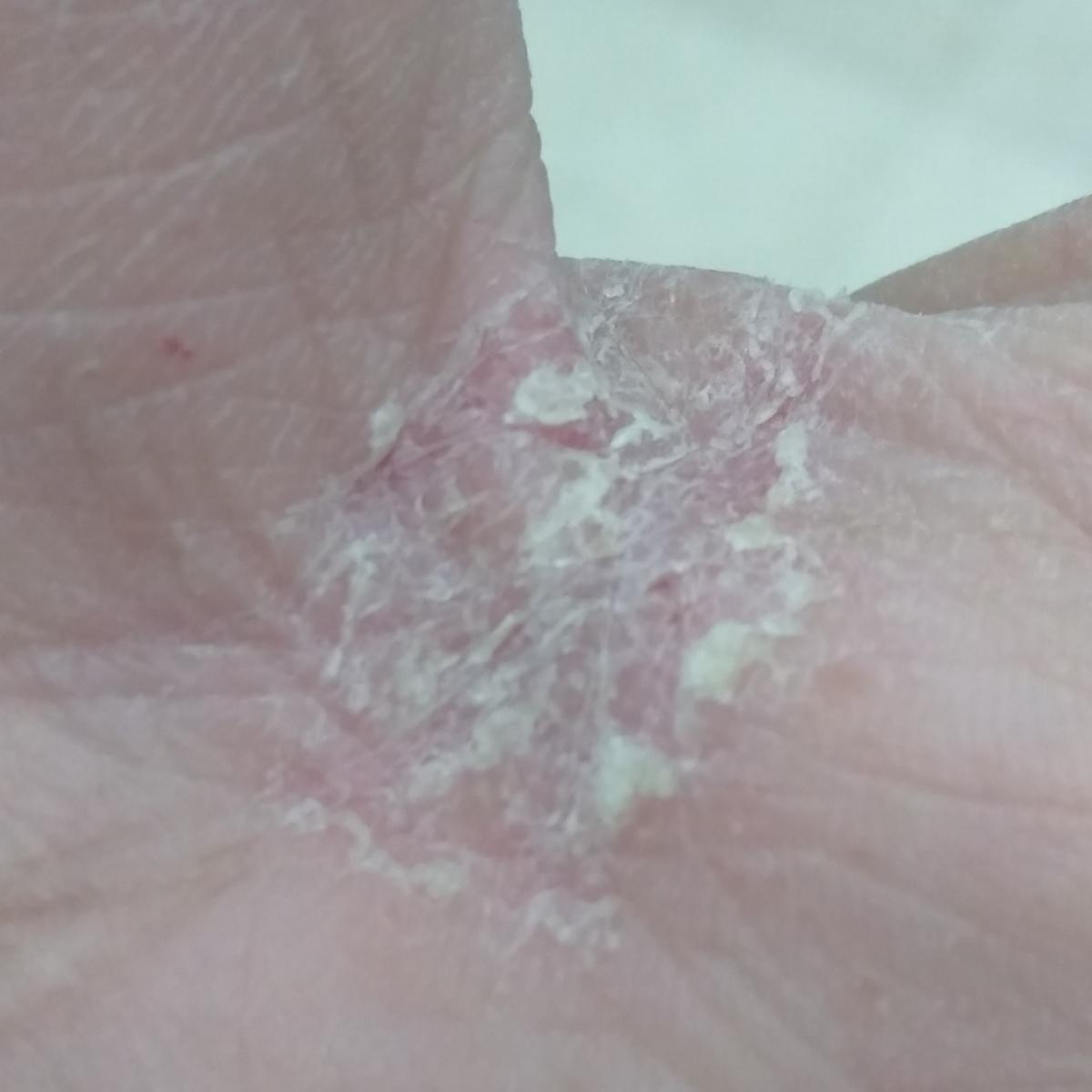
Shingles / pedis
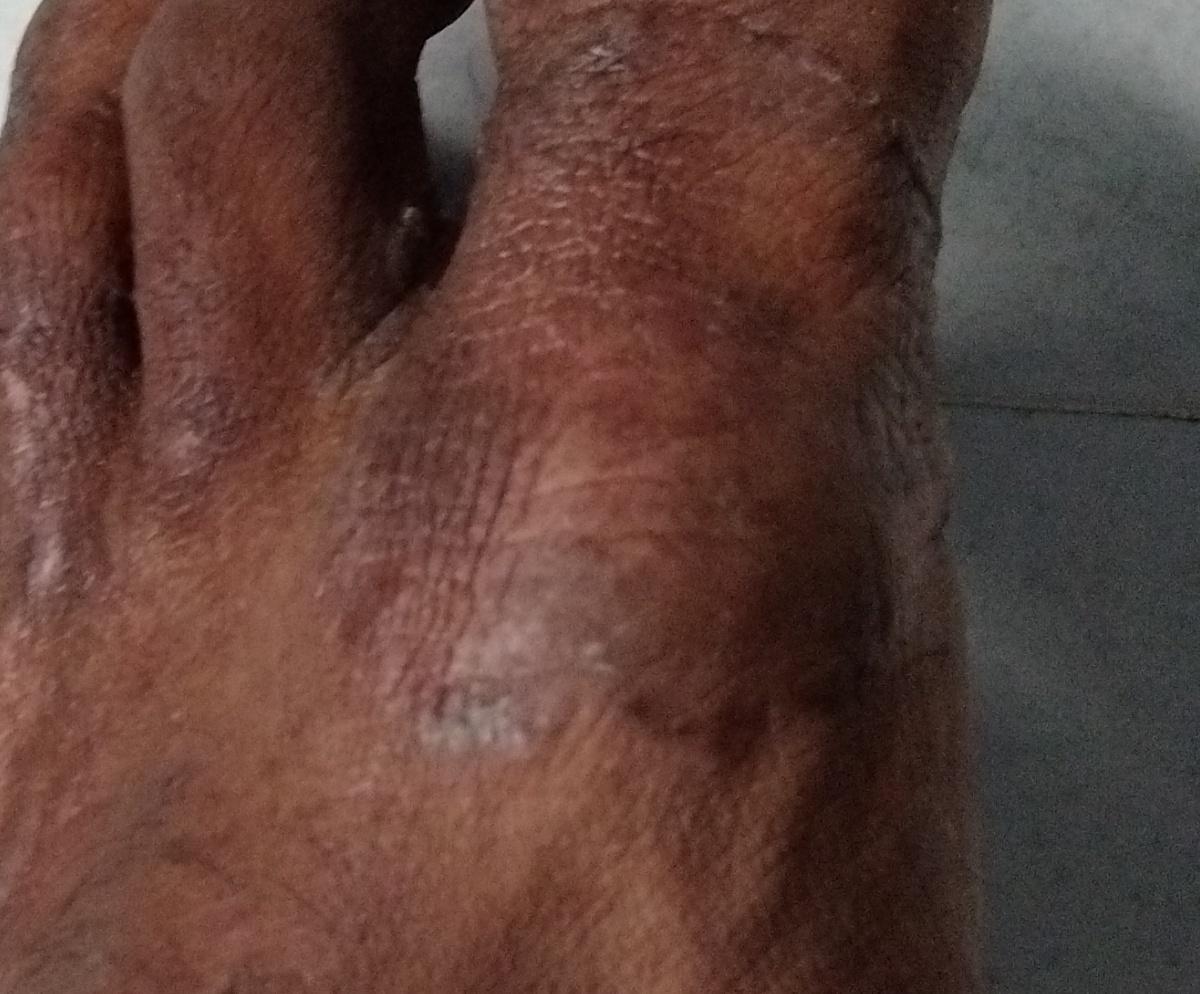
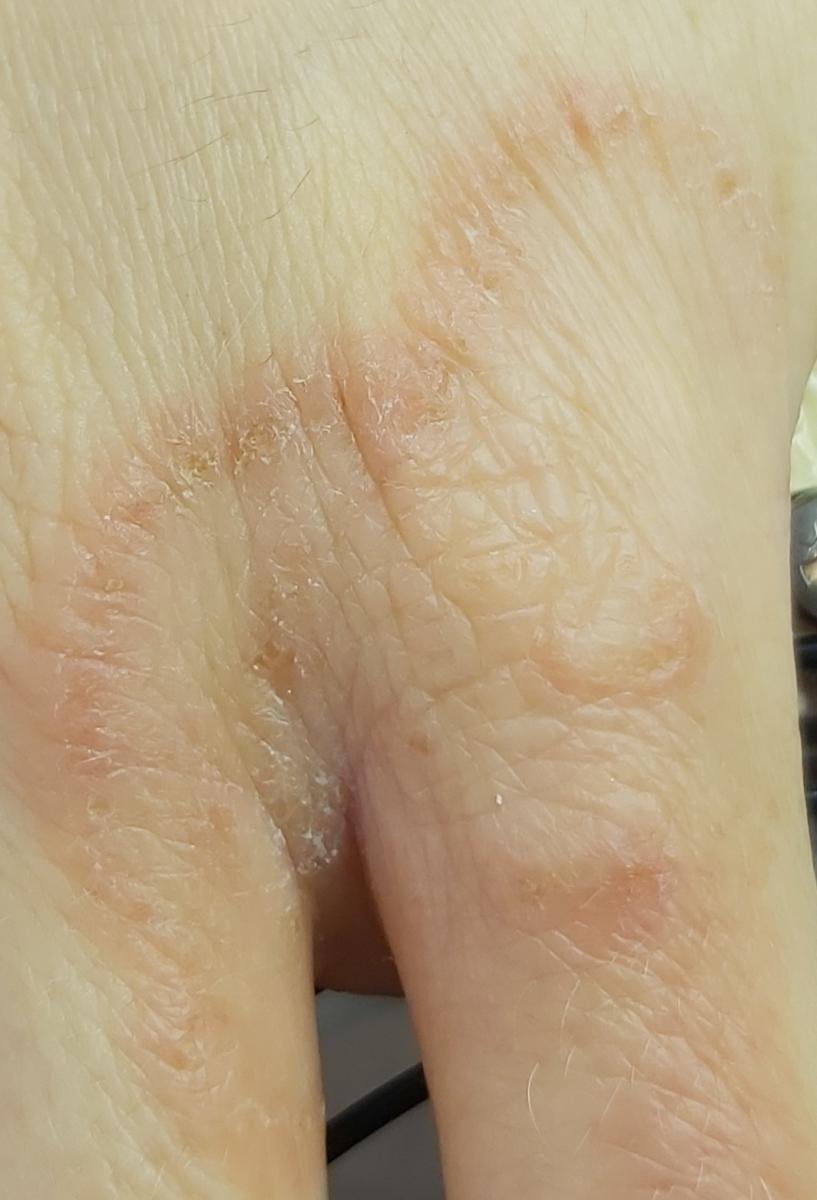
Fungal lesions of the palmar and plantar surfaces and interdigital spaces. It is the most common dermatomycosis worldwide.
The most common pathogens are Tr. rubrum, rare cases: Tr. mentagrophytes, E. flocossum.
Clinical views
Latent type – represented by mucous peeling in the folds of the palms and soles without inflammation, itching and thickening of the skin.
Chronic hyperkeratotic type (“mocassin” type) – affects the soles, lateral and medial sides of the feet: the skin is dry, covered with pityriasis scales with areas of hyperkeratosis, cracks, itching can be expressed.
Interdigital type (chronic intertriginous type, “athletic foot”) – affects the interdigital spaces of the feet, especially between the three lateral toes. Manifested by itchy erythema, peeling, painful cracks between the toes. An unpleasant odor may appear, spread to the soles or the back of the foot.
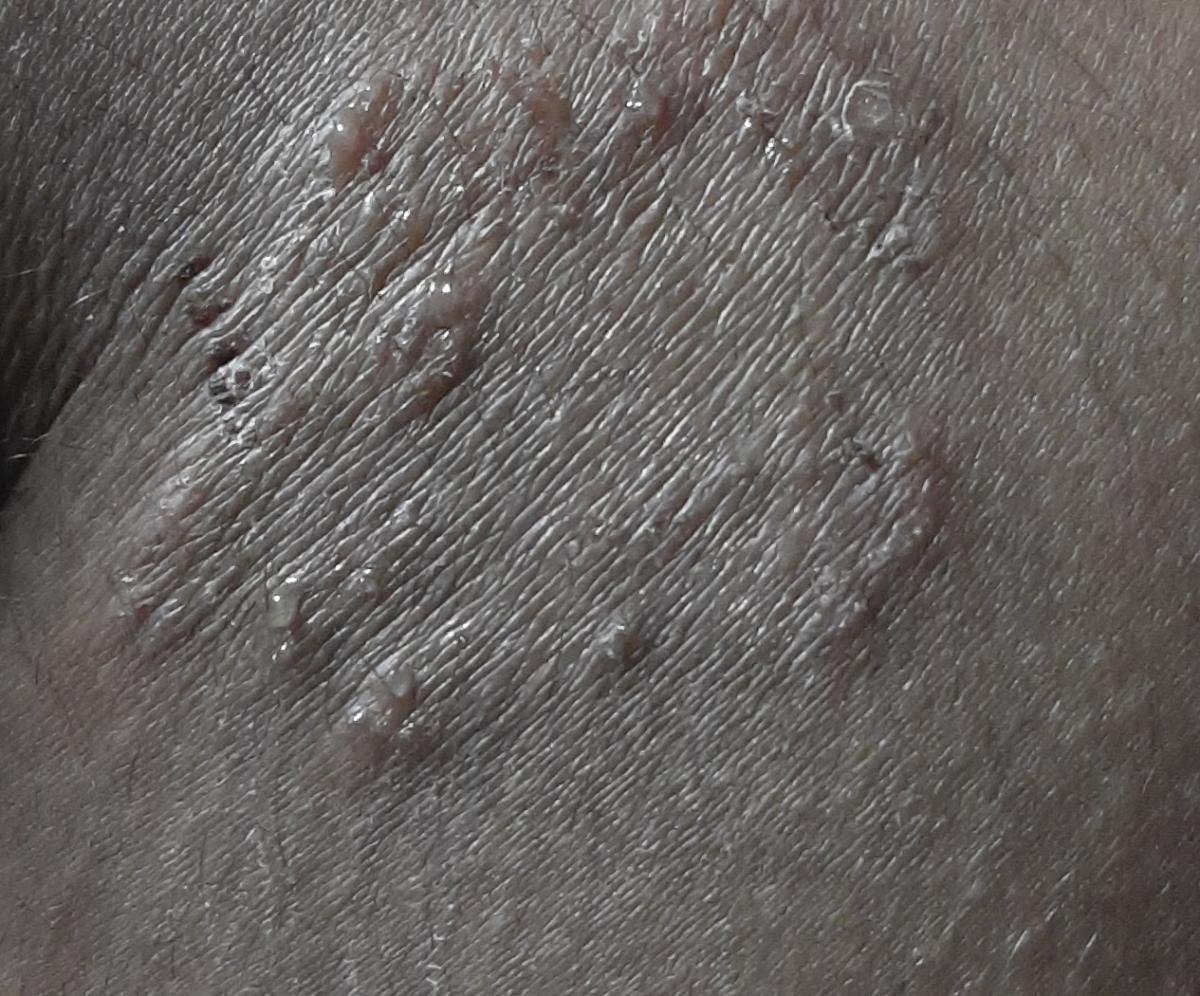
Vesiculo-bullous type (dyshidrotic) – manifested by tense vesicles with a diameter of 2-3 mm, rarely – vesiculopustules and blisters on the skin of the soles and peri-plantar space.
Acute ulcerative type is a complication of the interdigital or vesicular-bullous type with a secondary infection, most often caused by gram-negative microorganisms. Causes the formation of vesiculopustules and extensive festering ulceration on the plantar surface. The condition is often accompanied by cellulitis, lymphangitis, lymphadenopathy, and fever.
Tinea cruris
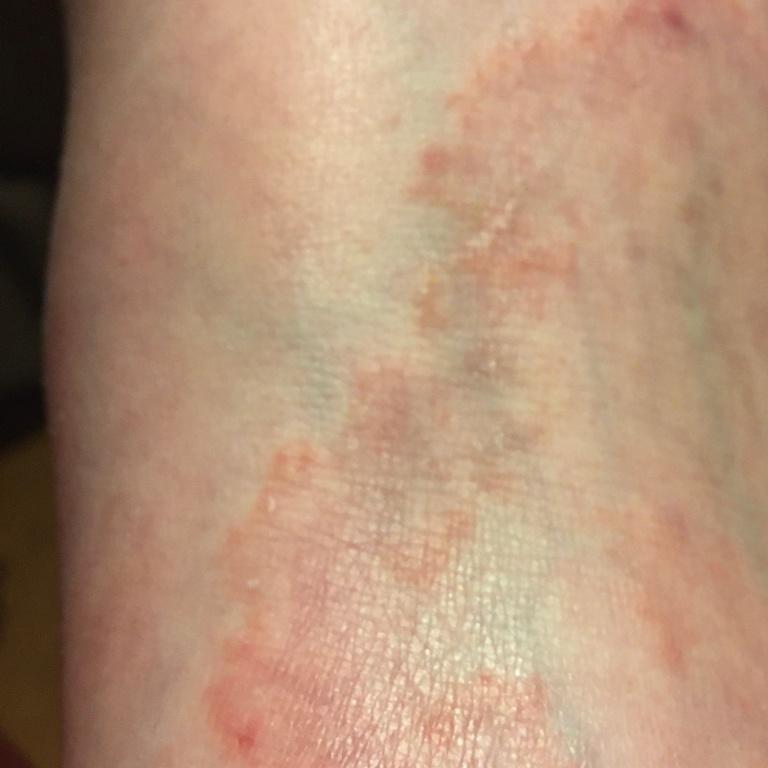
Dermatophytic infection affecting the groin folds.
Typical location: intergluteal, groin folds, inner thighs, pubic region.
Pathogens: the most common and specific – Epidermophyton flocossum, less often – Trichophyton rubrum.
Clinical picture
Mycosis of folds usually manifests itself as multiple erythematous papullovesicles with well-defined convex borders. Itching is common, as is pain with maceration and secondary infection.
Skin candidiasis
Candidiasis is a group of diseases caused by yeast-like fungi of the genus Candida. Unlike molds, Candida forms a pseudomycelium.
The most common causative agent of candidiasis – Candida albicans – a conditionally pathogenic microorganism, saprophyte, is present as a commensal organism in the vaginal mucosa in 20-25% of healthy women who do not present complaints, also colonizes in the oropharynx in 50% of healthy individuals, it is also possible to isolate Candida albicans in intertriginous areas of healthy people.
Epidemiology: infection is possible through direct contact, sexually, through household items. The most likely reason is the activation of endogenous infection due to predisposing factors:
- Immunodeficiencies (HIV, hyperimmunoglobulinemia E, chronic granulomatous disease, etc.);
- Nutritional factors (vitamin deficiency, general malnutrition, iron deficiency);
- Endocrinopathies (diabetes, obesity, thyroid disease, etc.);
- Taking certain medications (immunosuppressants, cytostatics, steroids, antibiotics, etc.);
- Hot and humid environment, skin trauma, dentures, tight clothing, etc.
Clinical manifestations
Cutaneous candidiasis
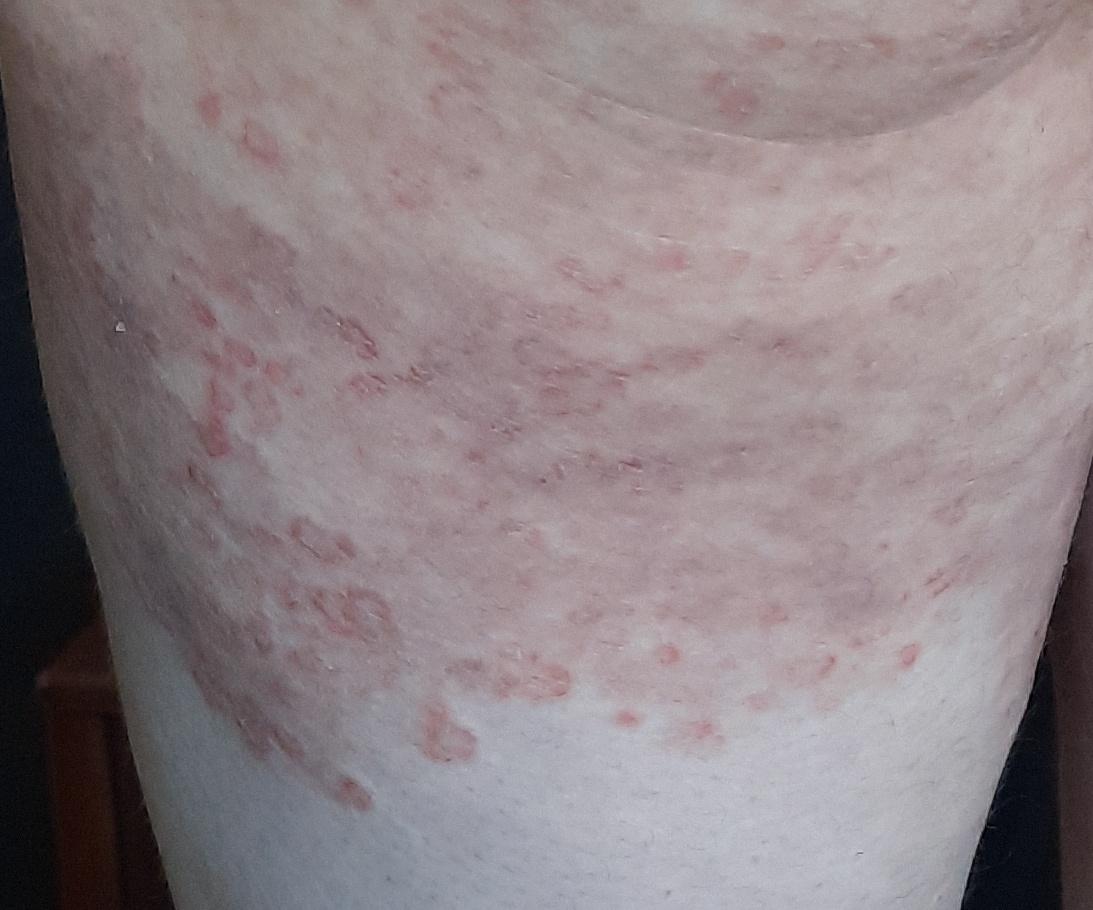
C. albicans tends to colonize skin folds: inguinal, axillary, submammary, intergluteal, interdigital, diaper area.
It looks like itchy, erythematous, macerated “flaming” spots (sometimes – erosive papules) with satellite vesiculopustular, easily turning into erosion. A special type is prickly heat, which affects the back of bedridden patients and looks like isolated vesiculopustular containing yeast.
Disseminated candidiasis
Disseminated candidiasis – candidal sepsis (hematogenous spread). Fungi of the genus Candida can get hematogenous access from the oropharynx or gastrointestinal tract, if the function of the mucous barrier is impaired.
With disseminated candidiasis, internal organs are affected. An increase in body temperature and a violation of the general condition are often observed.
Some patients may also have skin lesions: erythematous papules 0.5–1.0 cm in size with a hemorrhagic or pustular center, and necrotic foci may appear. The lesions are located on the trunk and limbs, the number of rashes varies.
Diagnostics
- Clinical picture;
- Microscopy of samples (scraping) from the skin, treated with 10% KOH and stained before examination: identification of oval budding cells, elongated filamentous cells, connected end-to-end (pseudohyphae);
- Cultivation on Sabouraud agar supplemented with antibiotics: whitish mucoid colonies grow within 2–5 days.
Treatment
For each type of candidiasis, there are affordable and effective treatments.
With local damage (if the immune status is not compromised), apply:
- Creams, ointments, solutions with drugs such as nystatin, levorin or natamycin, applied 1-2 times a day for 1-2 weeks.
With a widespread process, ineffectiveness of local treatment, chronic course or immunodeficiency:
- Itraconazole 100 mg – 2 times a day for 1-2 weeks; or 200 mg – 2 times a day for 1 week;
- Fluconazole 150 mg – once a week (once or for 2-4 weeks); or 50 mg – 1 time per day for 1-2 weeks;
- Ketoconazole 200 mg – 1 time per day for 1-2 weeks.
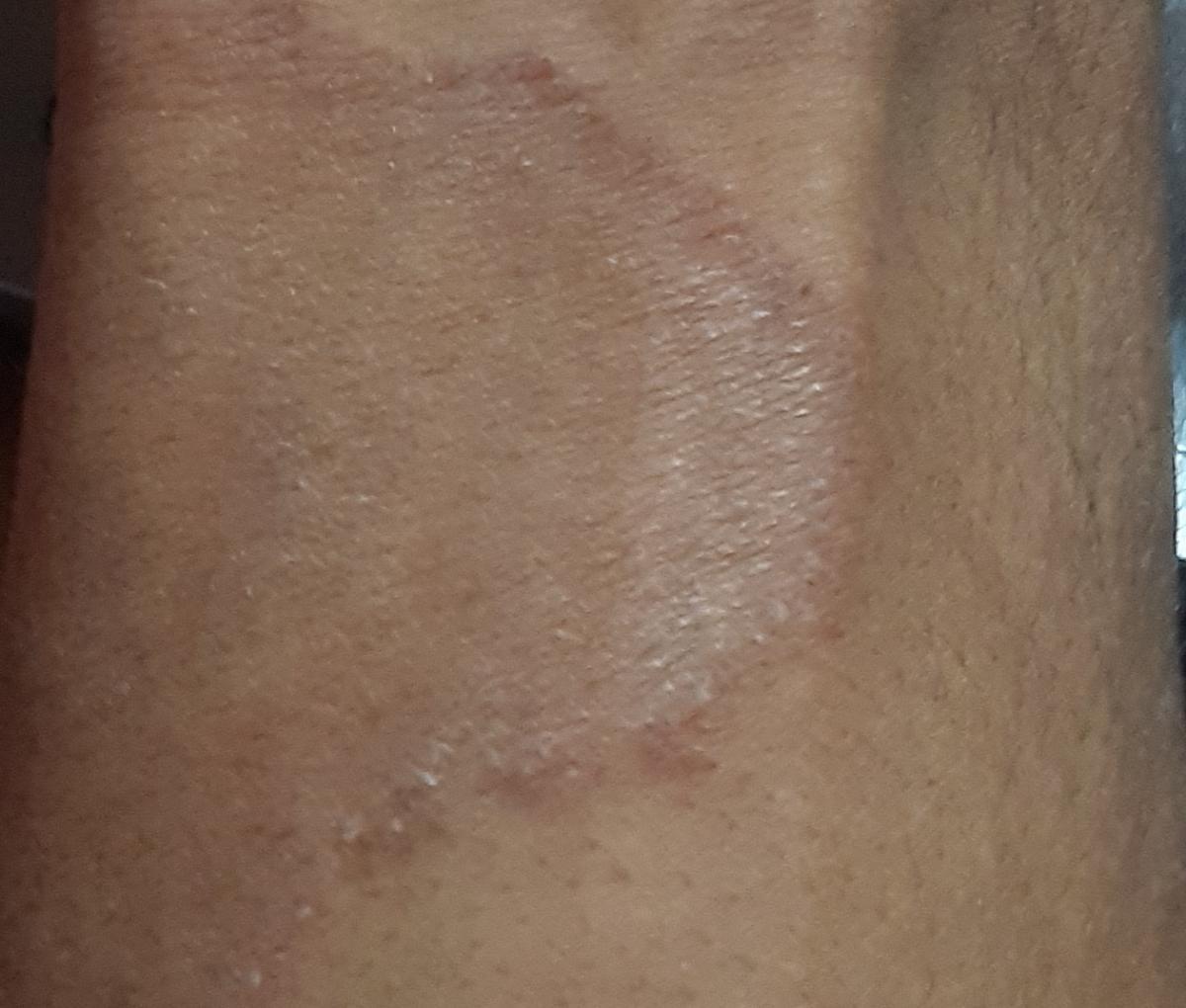
Tinea versicolor
Tinea versicolor is a chronic mycosis caused by fungi of the genus Malassezia, most commonly M. furfur. It can exist as a saprophyte – a yeast-like type that is a normal inhabitant of areas of the skin rich in sebum, and as a pathogen – an “activated” mold-like (mycelial) type that causes tinea versicolor.
Factors responsible for mycelium transformation include warm, humid environments, oral contraceptive use, heredity, systemic corticosteroid use, Cushing’s disease, immunosuppression, hyperhidrosis, and undernutrition.
Clinical picture
The most common manifestations of tinea versicolor are flaky, pigmented (non-inflammatory) patches of pink, yellow, brown, coffee with milk. For dark-skinned people, it is lighter than the surrounding skin.
Location: chest, back, abdomen and proximal extremities. Less commonly, the face, scalp and genitals are affected; in severe cases, the process can spread to large areas.
Borders are clearly demarcated. The size of the spots is up to 1 cm, but they tend to merge, forming large lesions. The complaints presented are usually of an aesthetic nature. Moderate or no itching. After sunburn, secondary hypopigmentation (reversible) remains.
It can also present with itchy folliculitis in the back, chest, and sometimes extremities. Primary eruptions are perfollicular, erythematous, in the form of papules or pustules 2-3 mm in diameter. Only appropriate culture and KOH test can distinguish this infection from bacterial folliculitis.
Diagnostics
- Wood’s lamp – yellow or orange glow;
- KOH microscopy – identification of filamentous mycelium and spherical pseudomycelium (type of “meatballs-spaghetti”);
- Culture Sabouraud-medium – slimy creamy colonies.
Treatment
For the treatment of milder forms, antiseptics and antifungal agents are used in the form of shampoos, solutions or creams (ketoconazole, clotrimazole, terbinafine) 2 times a day for 2-4 weeks.
Severe therapy includes systemic itraconazole (100 mg twice a day) or fluconazole (50 mg once a day) or ketoconazole (200 mg twice a day) for 2-4 weeks.