Molluscum contagiosum is a benign, rising above the skin, with a characteristic appearance, a neoplasm of a viral nature. The causative agent is the molluscum contagiosum virus (MCV), which belongs to the group of smallpox viruses. Molluscum contagiosum (MC) is most often found in children and adolescents, although it also occurs in adults, especially when the latter have immunodeficiency conditions and diseases.
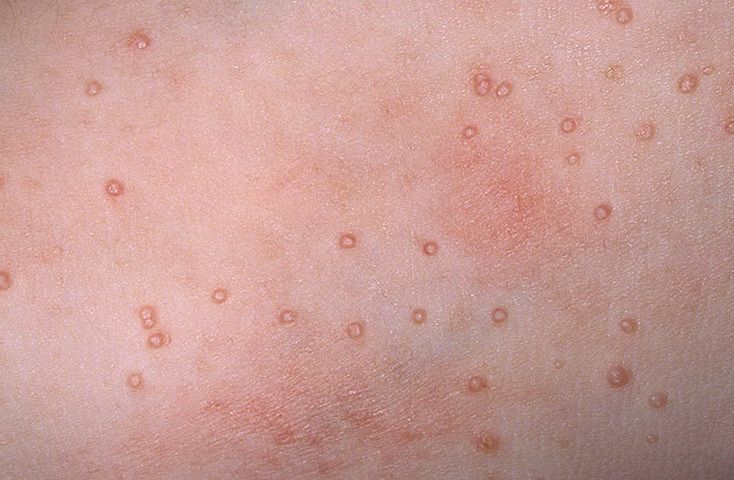
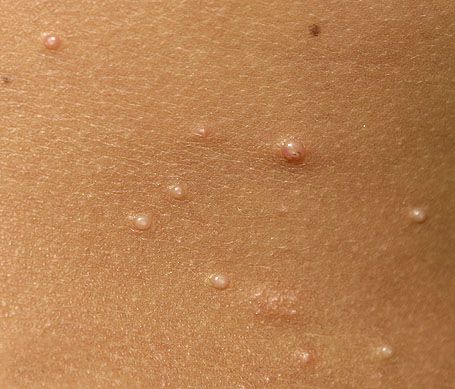
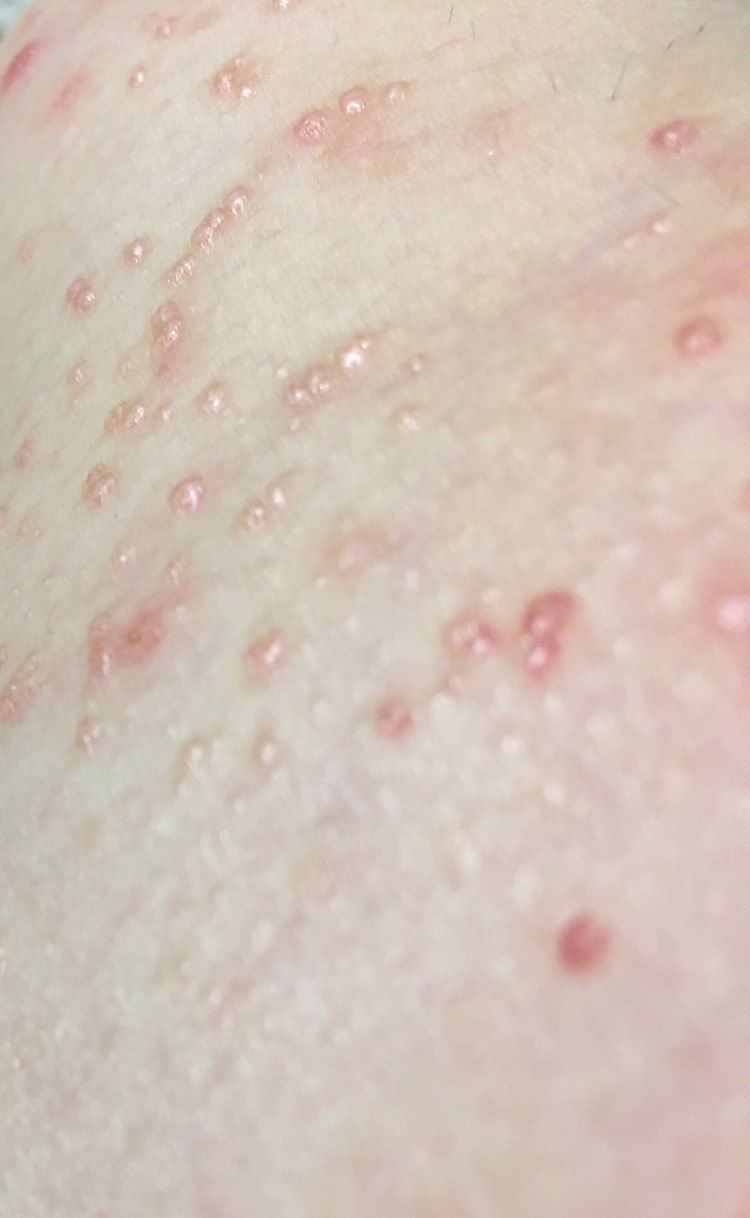
This type of neoplasm is characterized by multiplicity: usually, a group of neoplasms includes up to ten elements, sometimes a more massive lesion also occurs. With the immunity function preserved, spontaneous involution of the molluscum contagiosum may be observed, but this happens no earlier than after 6 months. Due to the high risk of further spread of MC, the presence of cosmetic discomfort, the risk of transmission to another person, treatment begins without waiting for spontaneous involution.
Predisposing factors
The cause of the appearance of molluscum contagiosum is the virus of the same name. Infection occurs by contact with the skin through household items, including through the contact of water with the virus (pool). If in children the most typical way of transferring the molluscum contagiosum virus is through contact with infected water and household items, in adults, transmission often occurs through sexual contact (with close contact of the skin). These infection paths also determine the most frequent location of molluscum contagiosum in different age groups.
Predisposing factors, which to varying degrees can increase the risk of neoplasms, include:
- Immunodeficiency states;
- Severe infectious diseases;
- Poor personal hygiene;
- Chronic skin lesions (like entrance gates for MCV).
Diagnostics
The diagnosis of molluscum contagiosum is based on anamnesis, a clinical examination, which includes a routine examination of the formation and dermatoscopy. With an unclear or ambiguous interpretation of the nature of the skin neoplasm, as well as with the identification of suspicions regarding malignancy, a biopsy (excision, complete removal of the neoplasm) can be performed.
Symptoms
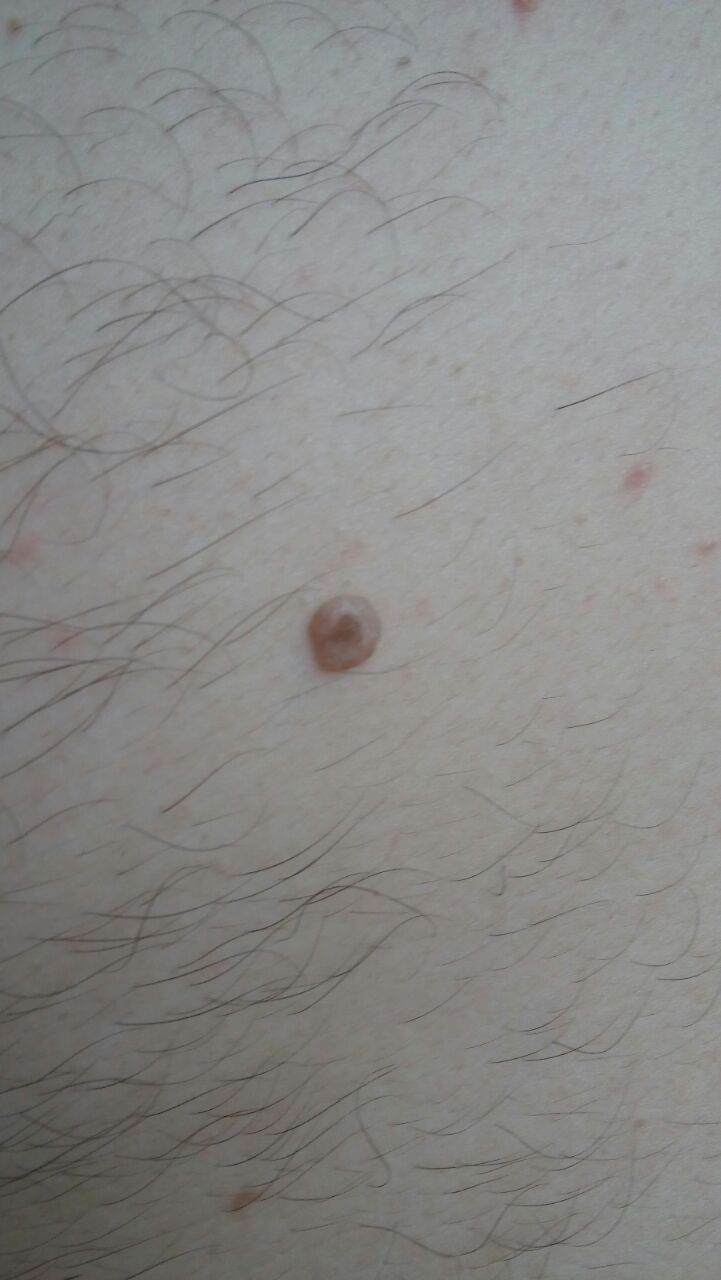
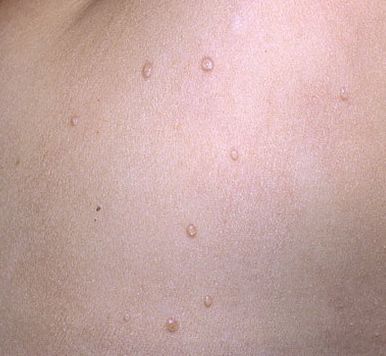
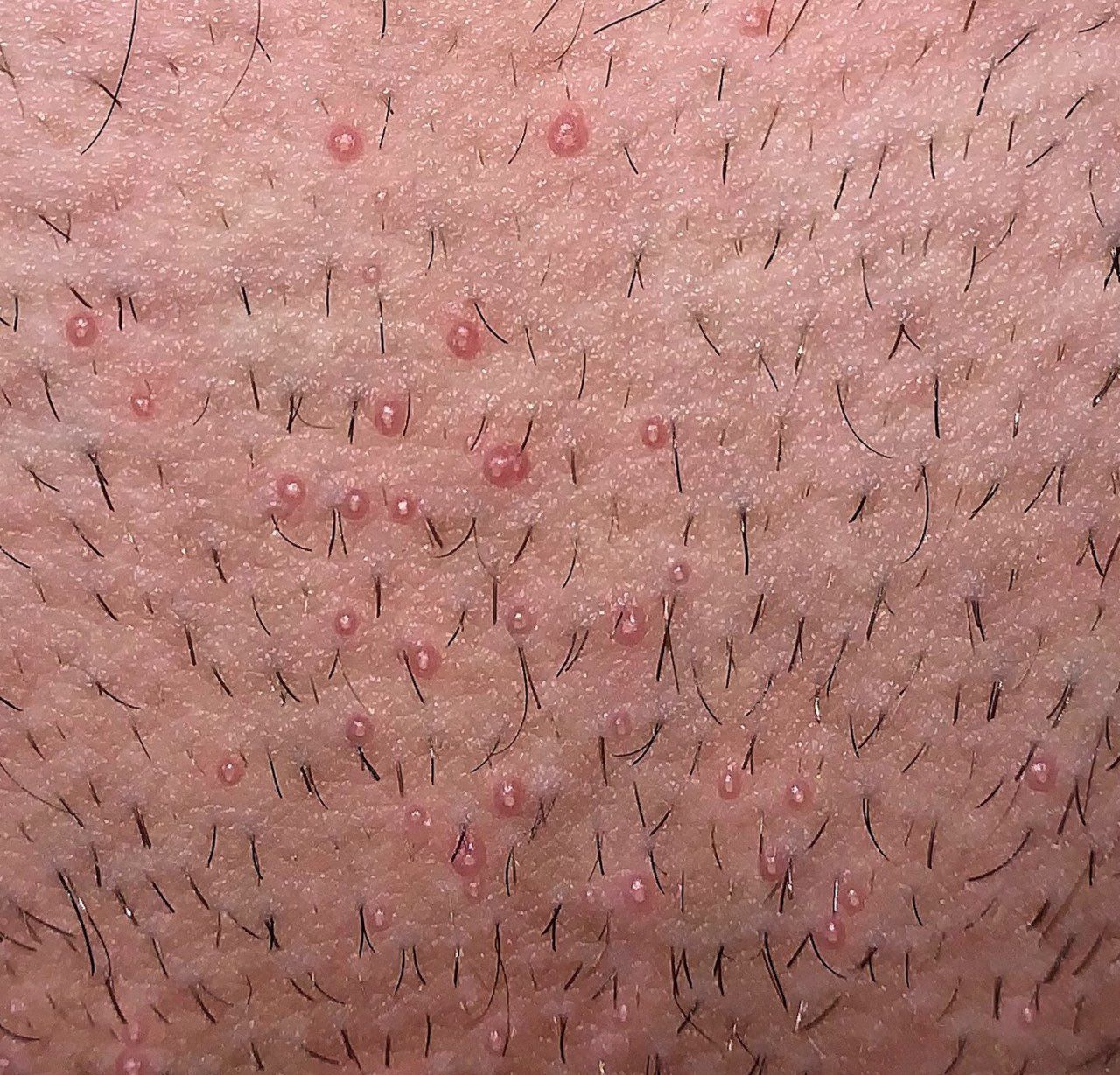
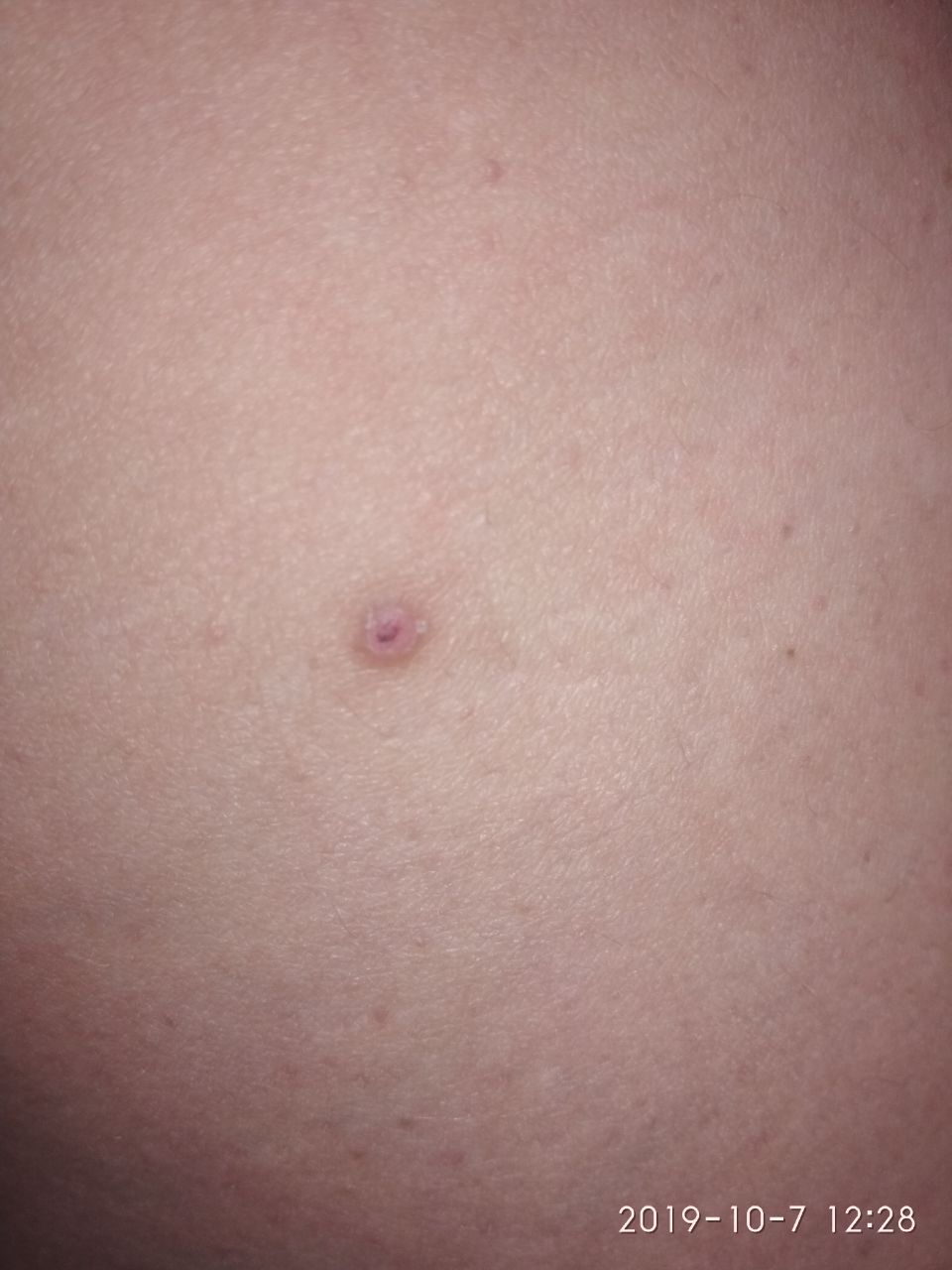
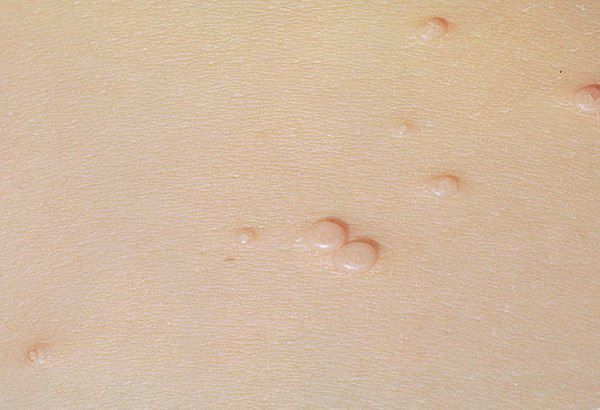
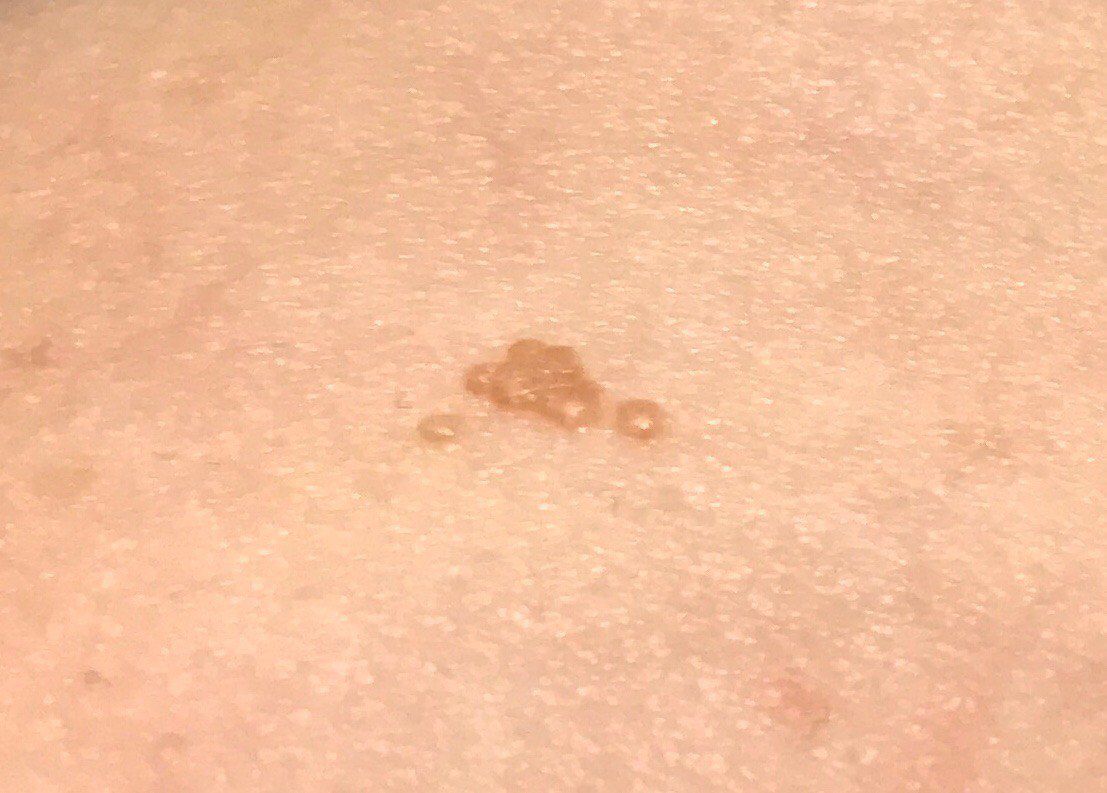
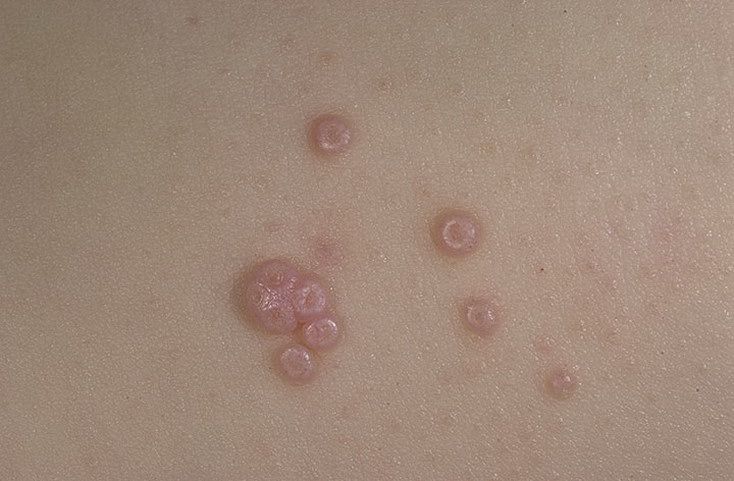
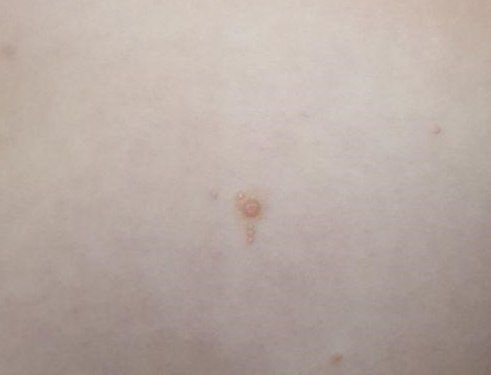
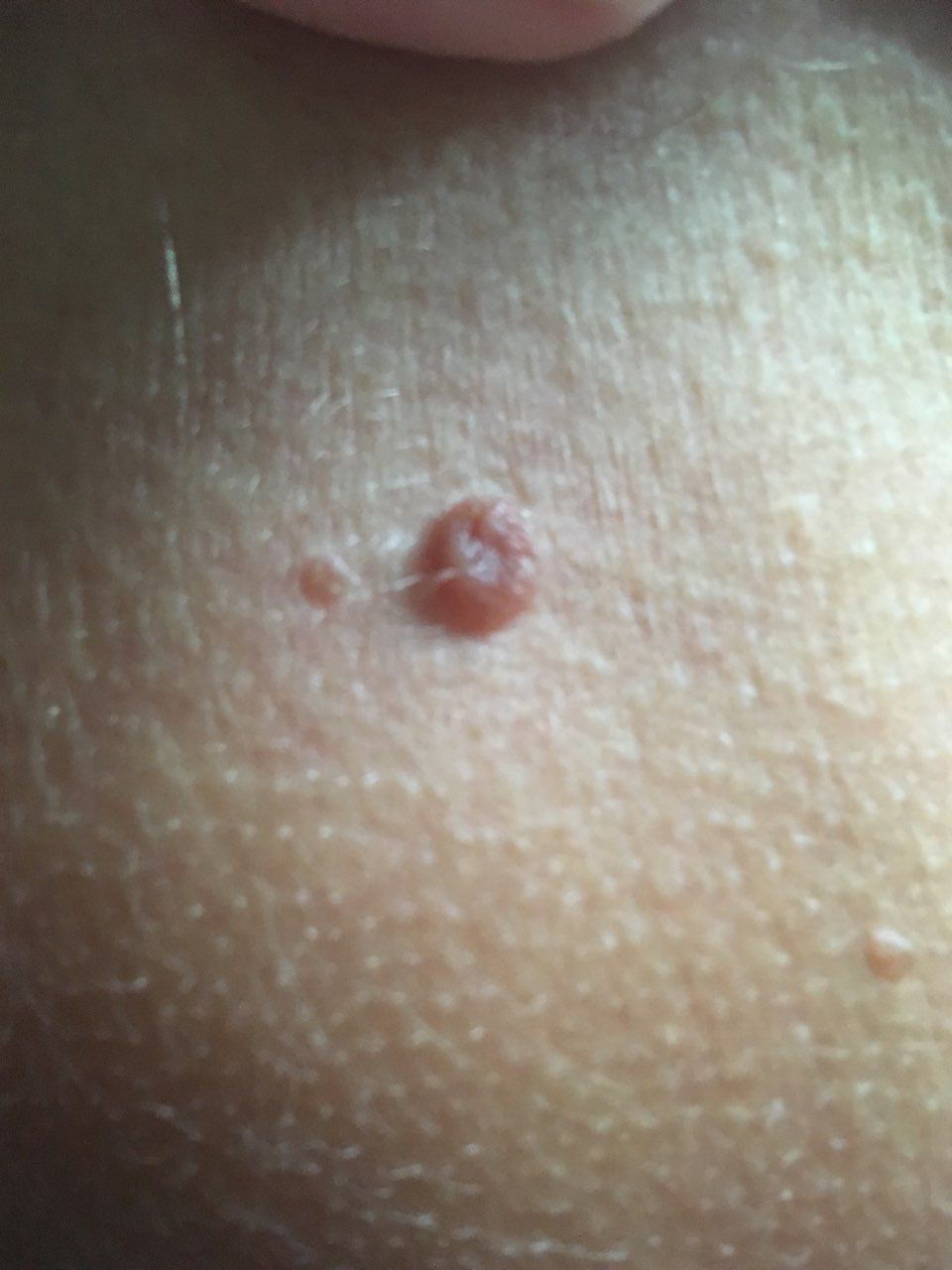
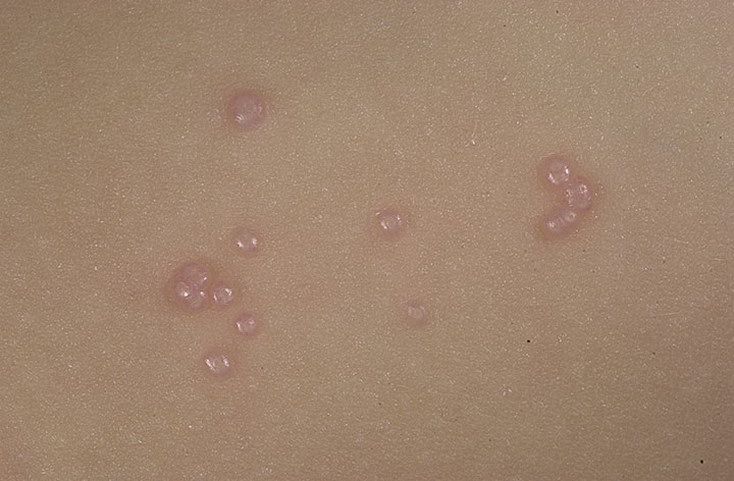
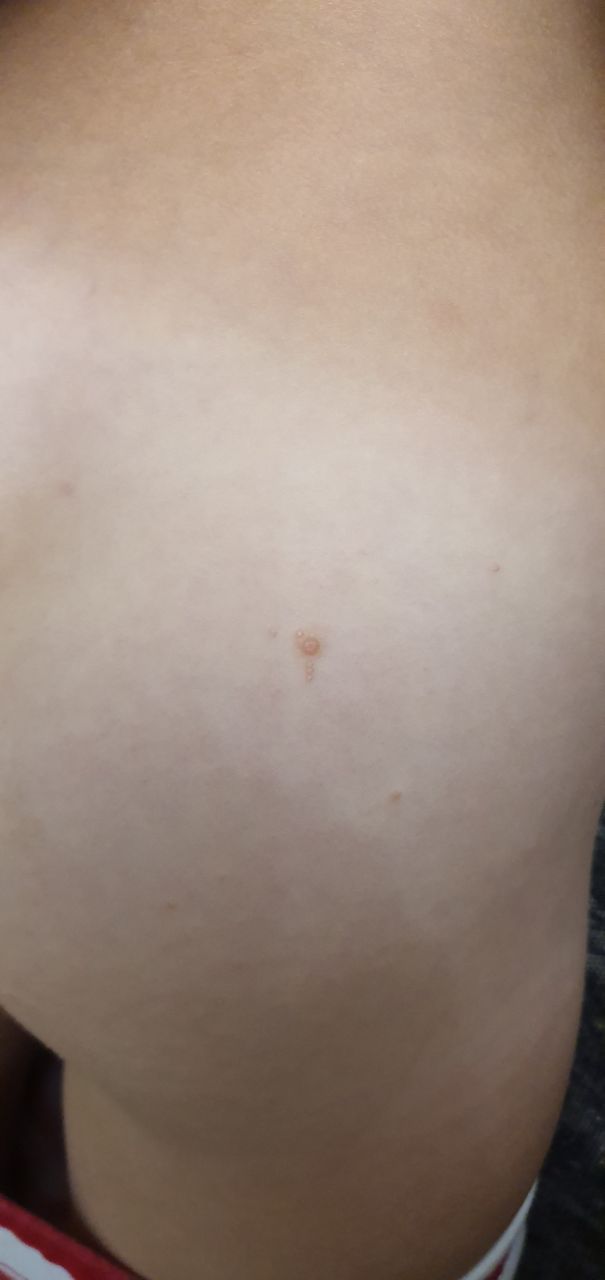
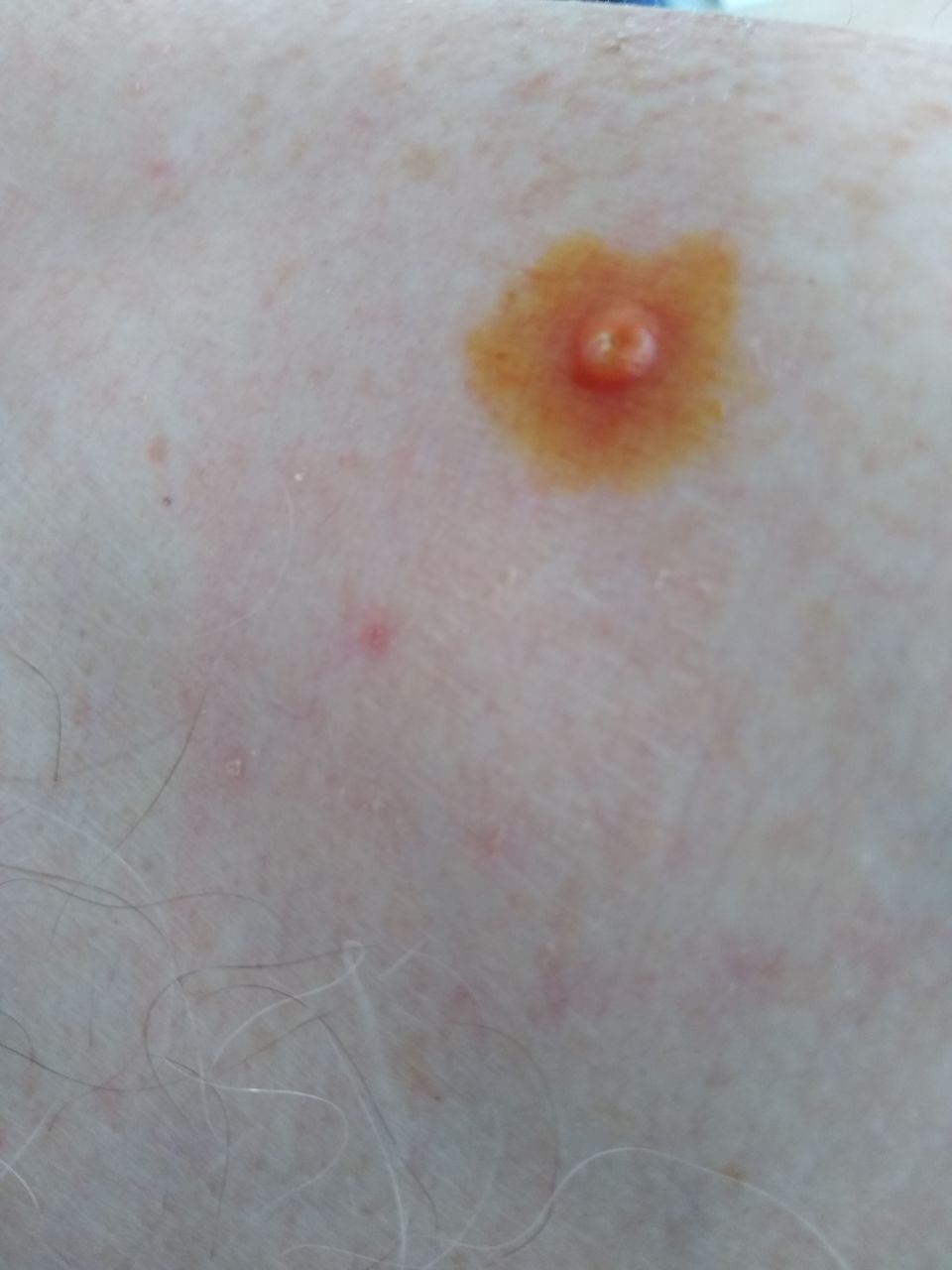
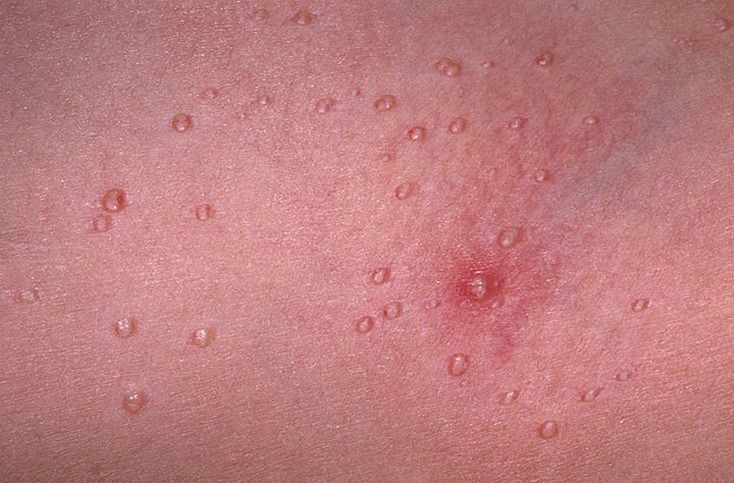
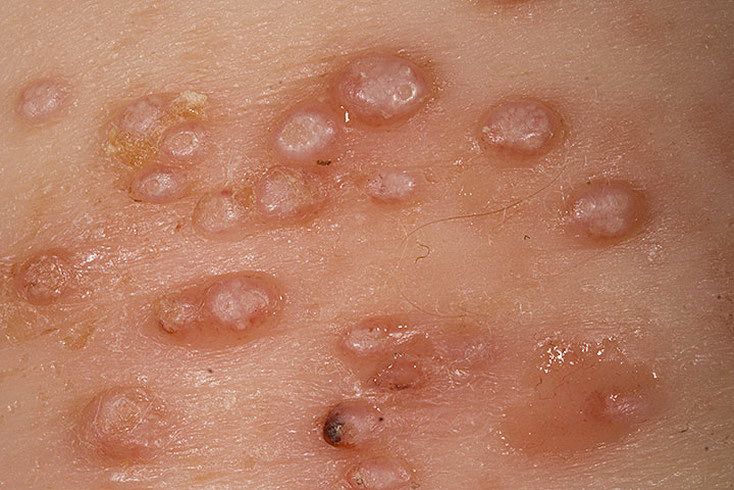
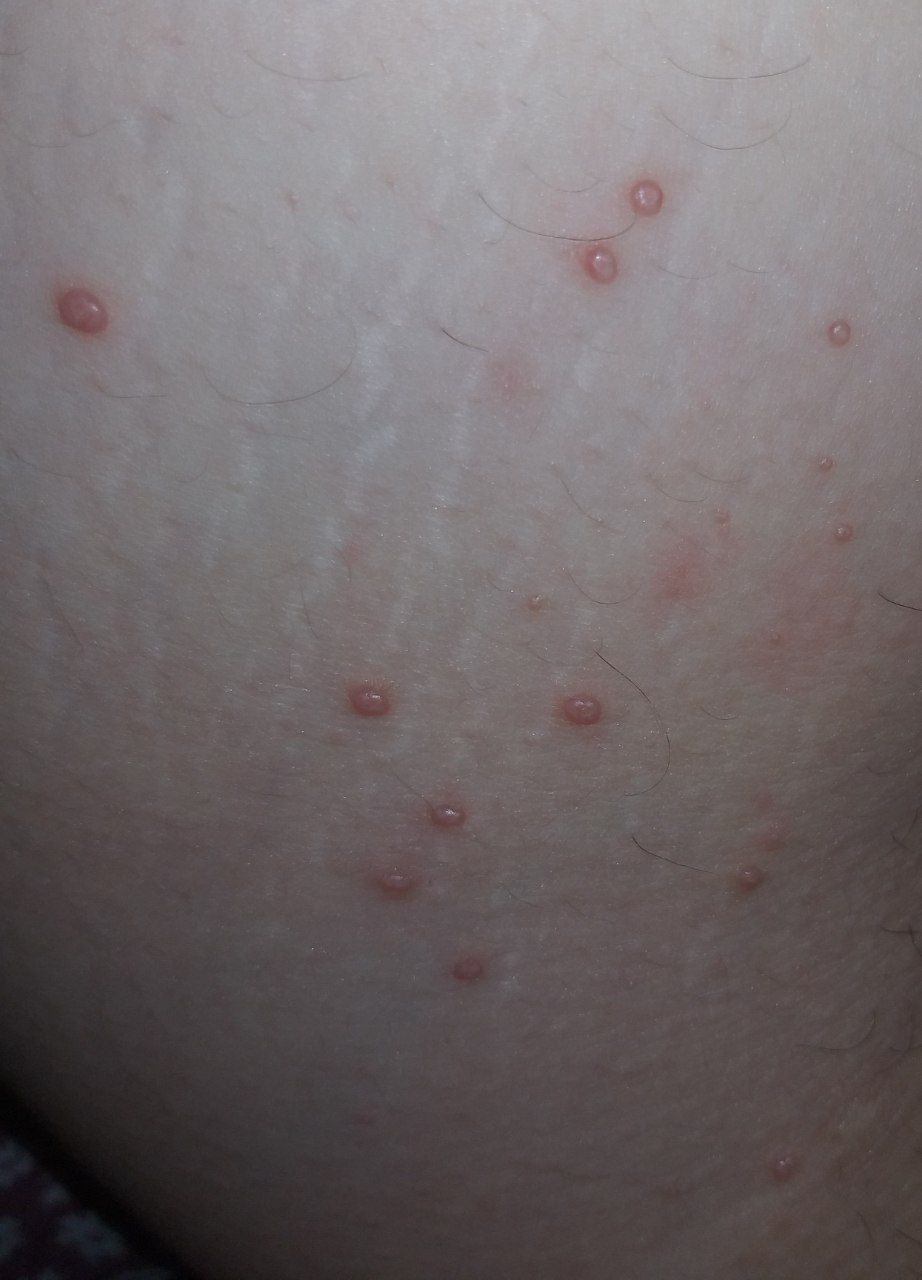
A visual examination of a molluscum contagiosum determines a dome-shaped formation rising above the skin. The surface is smooth, in the center there is an umbilical depression, a “dimple”, often filled with a structureless whitish content (cork). When squeezing the MC from the outside, the central plug begins to protrude in the form of a rod.
The boundaries of the molluscum contagiosum are clear and even. Body-color or slightly more intense pink. The cork in the center is whitish, light gray, but it is not always present (as a rule, it is found in later elements).
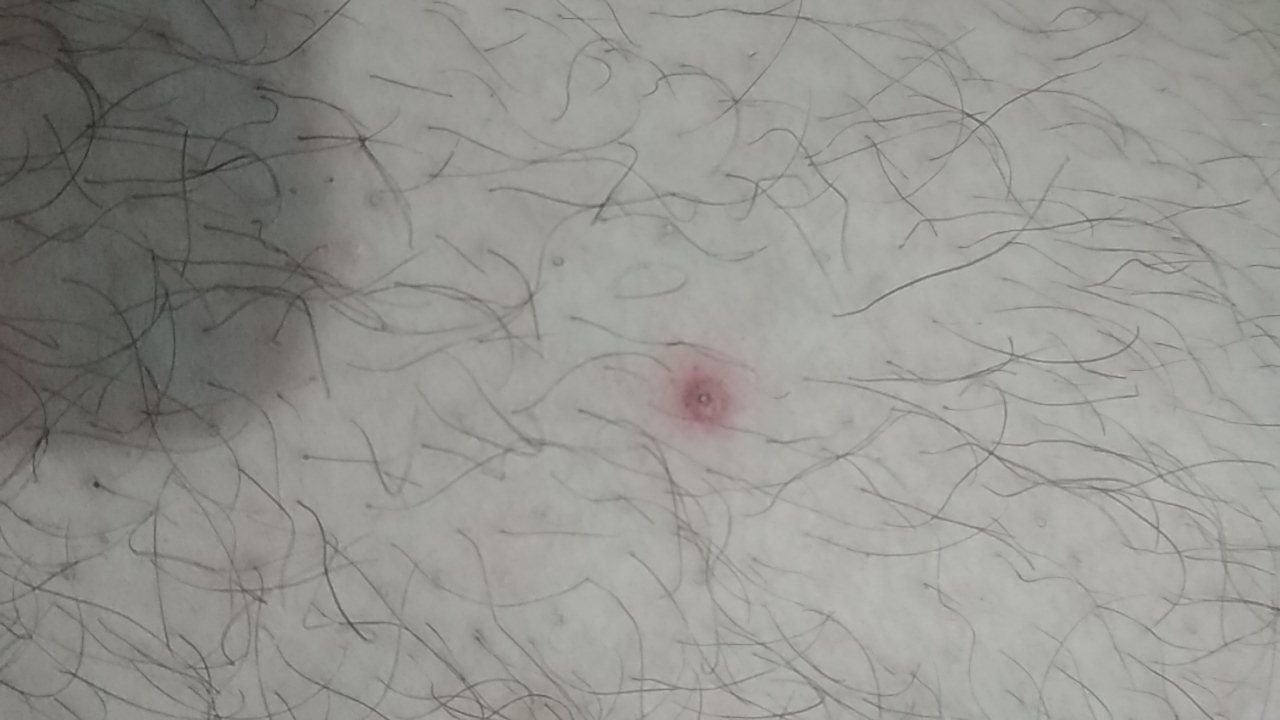
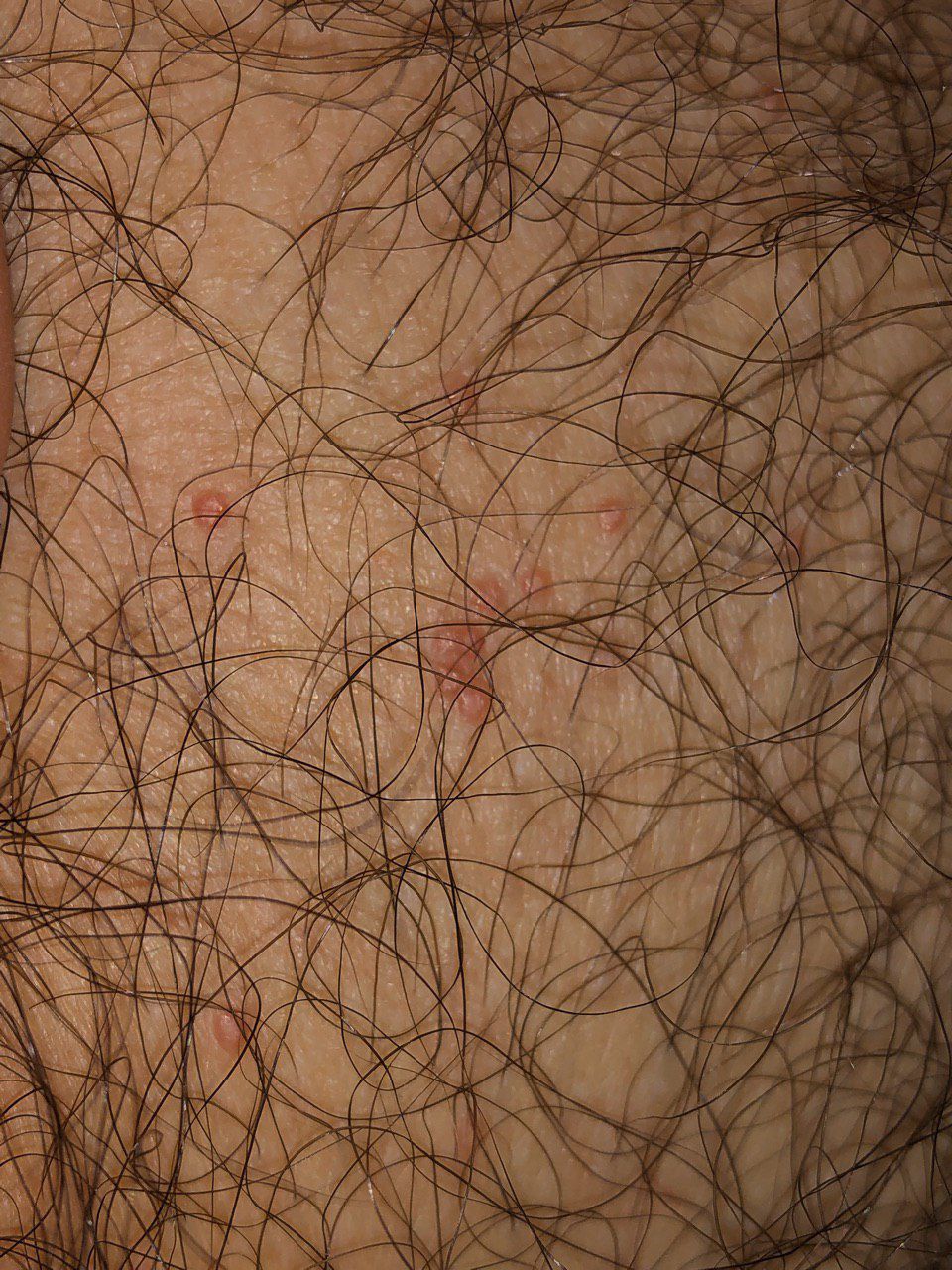
There is no hair growth on a molluscum contagiosum, but around – hair growth is not disturbed, so small molluscum contagiosum can be on the skin in areas of active hair growth, without changing their general appearance.
The sizes of the molluscum contagiosum are usually small: 2-5 mm, however, with a large number of elements, the latter can merge into larger conglomerates up to 10 mm or more.
On palpation, the molluscum contagiosum is slightly denser than normal skin, but over time, the elements become softer, corresponding to the consistency of the skin or even softer. Subjective sensations are also absent, sometimes itching is noted.
The molluscum contagiosum in children is located mainly on the extremities (with the exception of the palmar and plantar region) and face, less often on the trunk. For adults, the region of the lower third of the abdominal wall, inguinal region, pubic region, genital area, buttocks, less often the limbs, face are more characteristic.
Dermatoscopic Description
The following structures are visualized with dermatoscopy of molluscum contagiosum:
- Multiple rounded and oval-shaped structures with clear milky-white borders;
- The presence of cerebriform sinuous structures within the same formation;
- Multiple roundish structures of whitish and yellow color (polyglobular pattern of amorphous substance) are in the center;
- Radial unexpressed lines of a dotted or sinuous nature around an amorphous center (the so-called “crown”).
Differential diagnosis
Differential diagnosis is carried out with such neoplasms as:
- Papillomatous nevus;
- Nevus of the sebaceous glands;
- Dermatofibroma;
- Viral wart;
- Keratoacanthoma;
- Nodal form of basal cell carcinoma;
- Pigmentless melanoma.
Risks
From an oncological point of view, molluscum contagiosum is safe and does not carry an increased risk of malignancy. In the absence of an external effect on such a neoplasm (trauma, ultraviolet radiation, ionizing radiation), the risk of malignancy is comparable to the risk of a malignant tumor on unchanged skin. Signs of a possible tumor degeneration: rapid growth, increase in density, change in appearance, the appearance of subjective sensations.
From the standpoint of a viral disease, there are also no great dangers, since the molluscum contagiosum virus is located in the skin and does not spread to internal organs, respectively, without exerting a negative effect.
Molluscum contagiosum most represents a cosmetic problem and can cause psychological discomfort. The aggravation of the problem has the “contagiousness” of the disease.
Molluscum contagiosum, significantly protruding above the skin, is dangerous for its tendency to injure. As a result, there is bleeding, soreness, the resulting wound can become the entrance gate for another pathogenic microflora.
Given the viral nature of the molluscum contagiosum, with its multiple appearances, it is appropriate to talk about a decrease in the protective properties of immunity.
Tactics
In order to avoid the spread of neoplasms on the skin, as well as to prevent the transmission of the disease to another person, the molluscum contagiosum is subject to elimination from the body. To do this, you need to contact a dermatologist who will conduct the whole complex of diagnostic measures and plan treatment.
An immediate visit to a specialist is indicated if mechanical damage to the neoplasm, active exposure to ultraviolet or ionizing radiation, as well as if any changes in appearance or previously absent sensations have been noticed.
Dynamic monitoring of molluscum contagiosum, as a rule, is not used, with the exception of the patient’s refusal of treatment. In this case, photo fixation of the skin neoplasm with drawing up a map is of great value, which will make it possible to determine even minor changes in the appearance of the neoplasm in the future and record the appearance of new elements. With the progression of the disease (growth and increase in the number of mollusks) – a review of tactics with an explanation of the need for treatment.
Treatment
For the treatment of molluscum contagiosum, as a rule, less traumatic methods of removing elements are used:
- Laser removal;
- Cryodestruction with liquid nitrogen;
- Removal with a radio wave scalpel;
- Electrocoagulation;
- Local drug treatment (special pharmacy pharmaceuticals).
If it is impossible to conduct a less traumatic treatment, as well as in the presence of doubts as to the nature of the neoplasm, the usual surgical treatment is used by excision followed by histological examination of the obtained material.
When removing, it is important to comply with the rules that prevent the spread of the molluscum contagiosum virus through the skin.
Self-removal or “excretion” of MC cannot be performed due to the high risk of complications (bleeding, inflammatory processes), the risk of the virus spreading through the skin, and the impossibility of unambiguous independent determination of the nature of the removed neoplasm.
The patient is considered cured after removal of the last clam. However, due to the fact that the initial forms can be very small and difficult to distinguish from healthy skin, we can speak of a clear recovery and no risk of transmission of the virus one month after the end of treatment.
Immunity to molluscum contagiosum is not persistent, therefore ill persons have exactly the same probability of re-infection as people who have never experienced MC. Preventive measures to eliminate predisposing factors help reduce the likelihood of relapse.
Prevention
Prevention of the appearance of molluscum contagiosum consists of a gentle and careful attitude to the skin, timely treatment of infectious diseases, strengthening immunity, proper and high-quality personal hygiene, and maintaining a healthy lifestyle.
To exclude negative consequences and complications, it is necessary:
- Limitation of ultraviolet radiation of the corresponding area (tanning bed, solar tanning);
- The use of protective creams during periods of active sun;
- Exclusion of chronic skin trauma;
- Limitation or exclusion of ionizing radiation, occupational hazards;
- Compliance with safety measures when working with skin-damaging factors;
- Personal hygiene and basic awareness of skin tumors.
It also requires regular inspection of the skin, timely consultation with a specialist in case of any neoplasms detection.