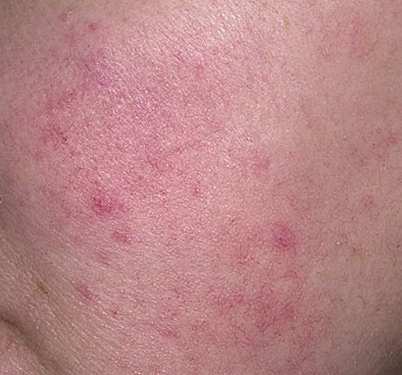
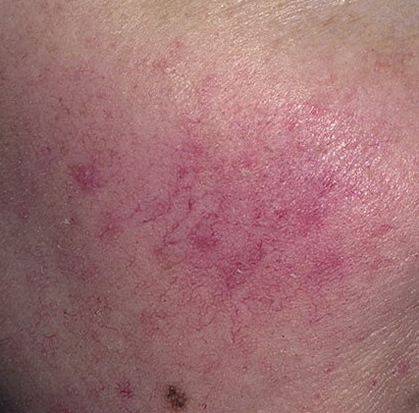
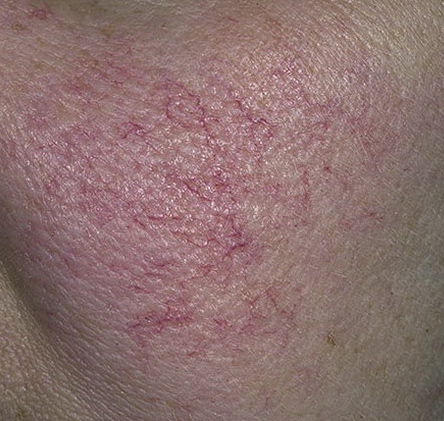
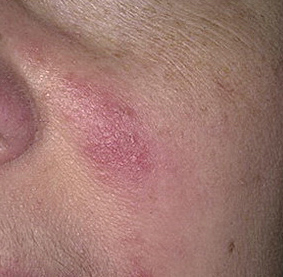
Rosacea is a chronic inflammatory skin disease associated with hyperreactivity of the facial capillaries and damage to the sebaceous glands and hair follicles. With rosacea, depending on the subtype and severity of the disease, such elements as skin hyperemia, telangiectasia, erythema, papules, pustules, rhinophyma appear. The localization of rosacea is the face.
Despite the fact that the clinical picture and location of rosacea is similar to acne, the first pathology has completely different mechanisms of appearance, cause-and-effect relationships, of course, and is an independent disease not associated with acne. At the same time, these two diseases can be present in one patient.
Rosacea usually occurs in middle age, starting at the age of 30, reaching a maximum manifestation in 40-50 years. This is why rosacea is also called adult acne. The prevalence of rosacea is observed mainly in fair-skinned people with 1-2 skin phototypes and occurs in 10% of the population.
The appearance of rosacea is associated with increased reactivity of the blood capillaries of the facial skin. In response to the stimulus, the capillaries expand, lose their tone, the blood flow rate slows down in them, and oxygen delivery to the tissues is disrupted. These conditions become favorable for the pathological reproduction of the natural microflora of the skin and the attachment of pathogenic microorganisms. A progressive inflammatory reaction leads to the appearance of edema and papulopustular rash of varying severity.
The listed factors can also be the primary link in the pathogenesis of rosacea, triggering a chain of pathological processes in the functioning of the capillary circulation of the facial skin with the subsequent addition of infection.
Diagnostics
Diagnosis of rosacea is based on history and clinical examination. A carefully collected anamnesis allows you to find out the time of the onset of the skin disease, the conditions, the course. Clinical examination reveals the typical elements characteristic of rosacea. If such a need arises, especially in the presence of suspicious and ambiguously interpreted elements or in case of unexpressed manifestations, dermatoscopy can be performed.
Careful diagnosis is necessary to correctly determine the severity of rosacea, as well as to maximize the identification of provoking factors. All this allows in the future to select an adequate treatment and individually form preventive measures.
Symptoms
The symptoms of rosacea depend on the severity of rosacea (phase, shape, subtype) of the disease. The clinical picture of rosacea in the classic version includes four subtypes, depending on the severity of symptoms:
- Erythematous-telangiectatic rosacea;
- Papulopustular rosacea;
- Phimous rosacea;
- Ophthalmic rosacea.
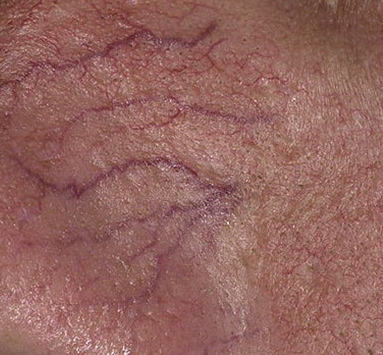
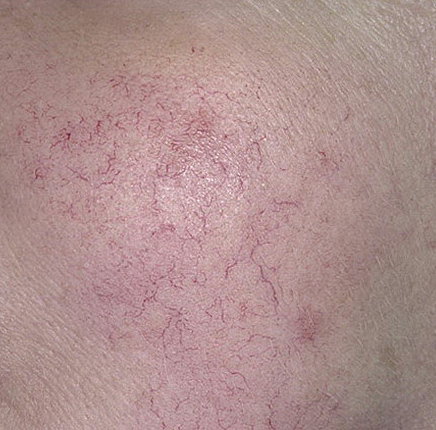
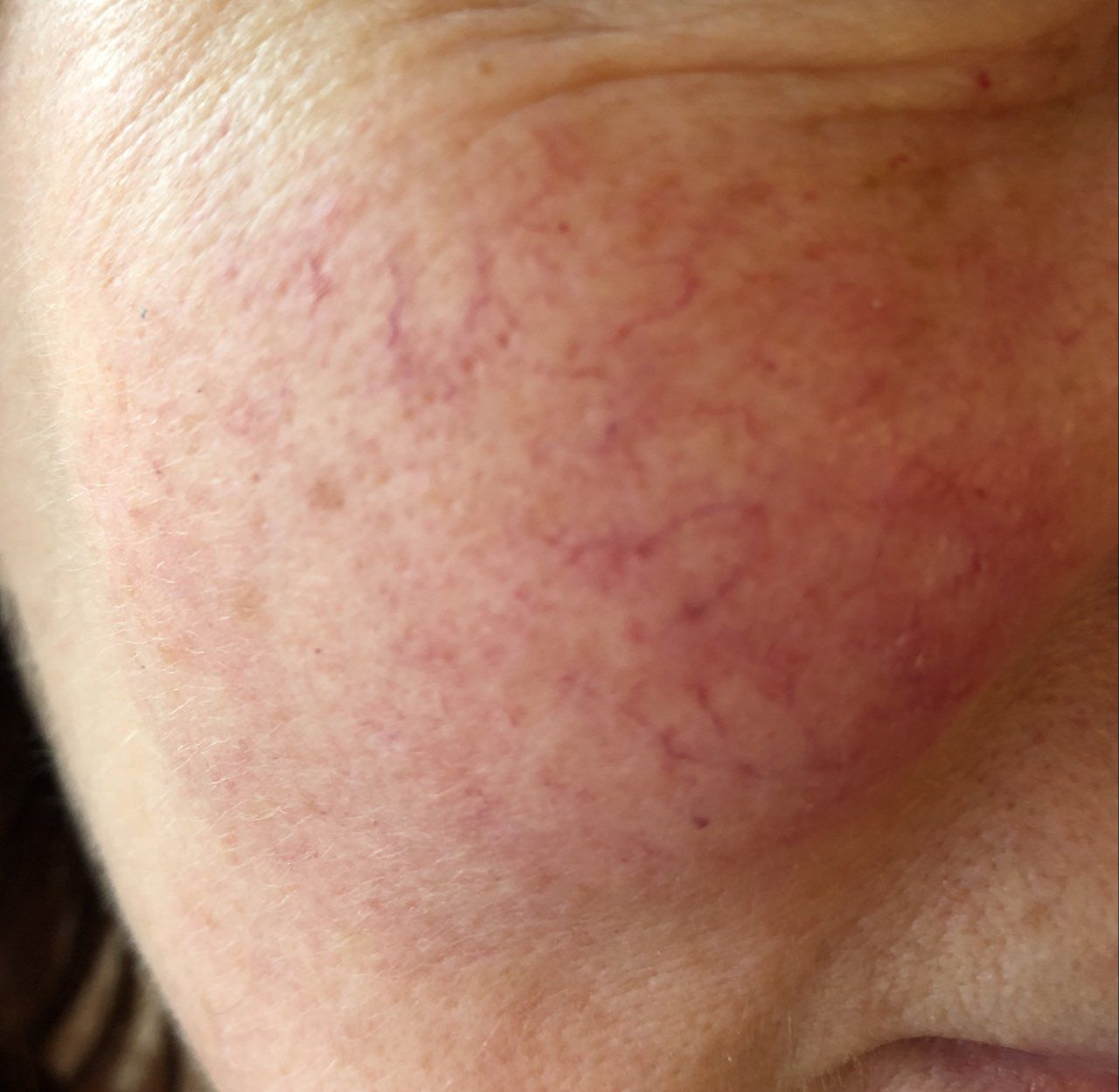
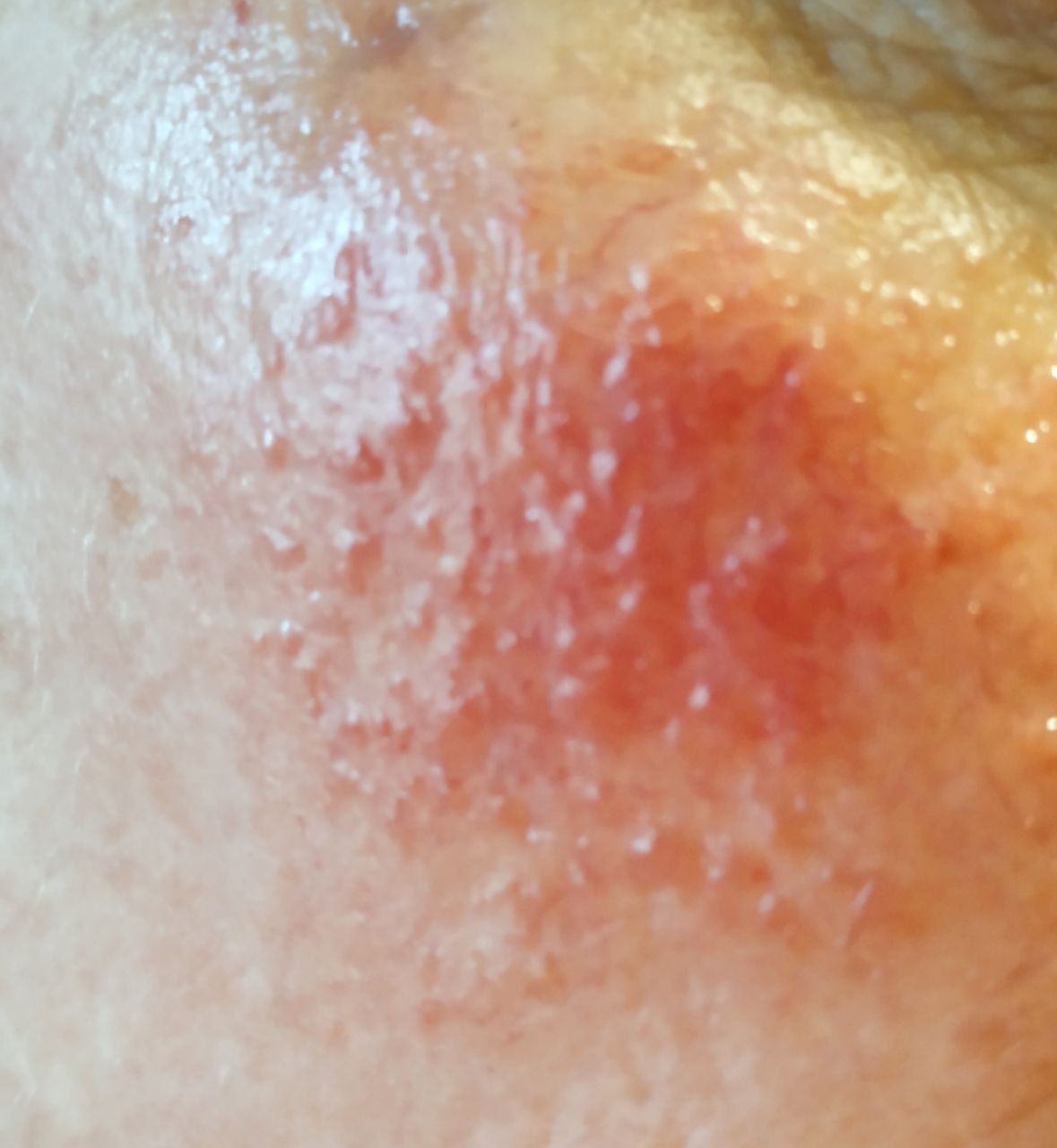
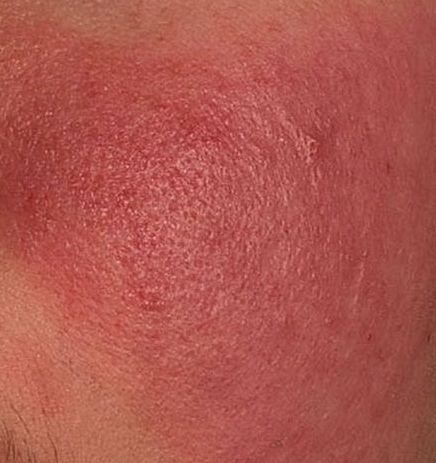
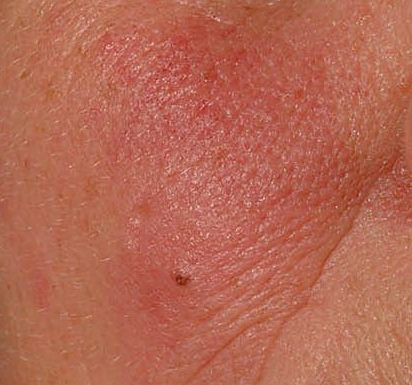
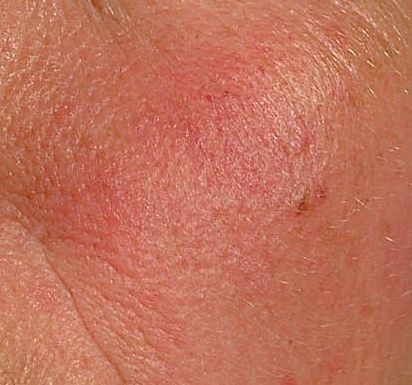
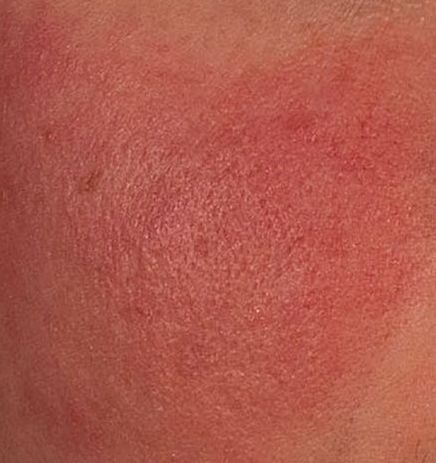
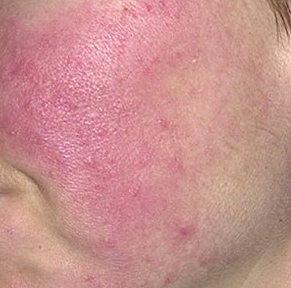
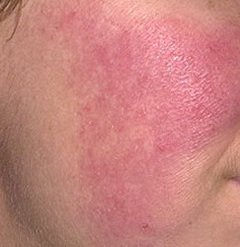
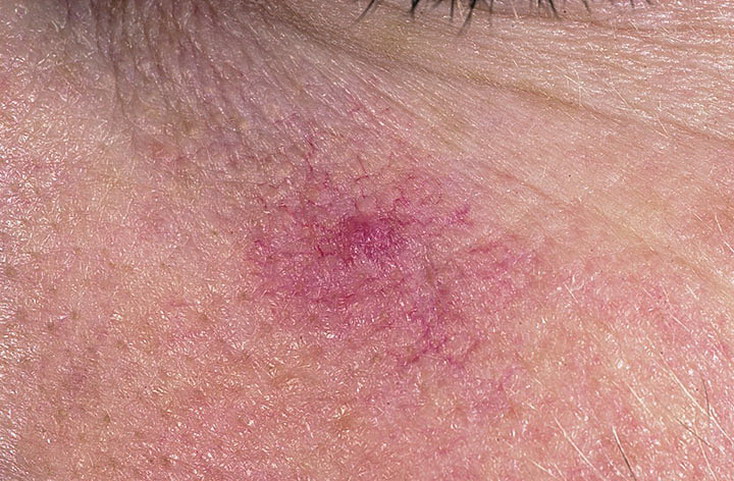
Erythematous-telangiectatic rosacea is characterized by flushing of the face (redness) in response to provoking factors, the so-called “erythema of shame”. At the onset of the disease, hot flashes pass without a trace, but over time, small bright red convoluted vascular capillaries – telangiectasias – remain on the skin after the hot flush, which over time becomes more and more, they become grouped, multiple and practically do not disappear. At this stage, the skin pattern is not changed, there may be a slight itching or just discomfort on the skin, especially during periods of hot flashes.
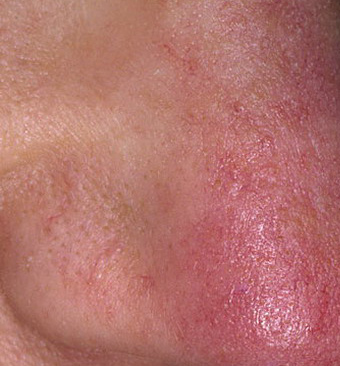
With erythematous rosacea, microcirculation disorders appear, difficulties in venous outflow of blood and, as a result, a decrease in the protective properties of the skin. This leads to the development of an inflammatory reaction and the formation of papulopustular rosacea, against the background of the erythema described above. The situation can be complicated by the addition of pathogenic microflora.
A papule is a common pimple with no content inside: a slightly elevated, pink-red or red, painful formation on contact with fuzzy boundaries. Their base diameter does not exceed 1-3 mm. A hyperemic skin reaction around the pustule can be up to 10 mm in diameter. In the presence of severe inflammation, the papule may be denser than normal skin. The surface of the skin looks healthy or slightly smoothed.
A pustule is a common pimple with whitish or yellow-tinged contents inside. It is slightly elevated, pink-red or red around the periphery and whitish in the center, painful on contact, with indistinct boundaries. The pustule is usually denser than the surrounding skin. The diameter at the base does not exceed 1-3 mm. A hyperemic skin reaction around the pustule can be up to 10 mm in diameter. The surface is usually smooth, especially in the center. When squeezed, the pustule is opened and structureless white contents are released from it.
Phimous rosacea is a pronounced hyperplasia of the soft tissues of the face in response to the inflammatory process: the skin acquires a purple-cyanotic hue, edema, rough tuberosity up to cyanotic nodes. The fusion of the nodes forms disfiguring infiltrates up to the deformation of the contours of the face.
Ophthalmic rosacea is the spread of rosacea of any severity to the eye area with damage to the eyelids and periorbital tissues. Occasionally, ophthalmic rosacea can be a precursor to rosacea in other areas of the face.
Differential diagnosis
Differential diagnosis is carried out with diseases such as:
- Different degrees of severity and forms of rosacea;
- Acne, including rashes, drug-induced acne;
- Dermatitis and dermatoses;
- Actinic keratosis;
-
Against the background of severe forms of rosacea, for example, rhinophyma or conglobate form of rosacea, differential diagnosis is performed with nodular forms of basal cell carcinoma and non-pigmented melanoma.
Risks
Rosacea does not pose a major threat to a person’s physical health. At the same time, the presence of this pathology may indicate the presence of some kind of rearrangements in the body: from physiological (such as puberty) to pathological (metabolic disorders, decreased immunity). Being a kind of mirror, a reflection of the internal state of the body, the appearance of rosacea cannot be ignored, it is necessary to conduct a deep search for the causes and provoking factors. This will contribute not only to the effective treatment of rosacea, but also to the timely search for other, possibly more serious diseases.
On the other hand, rosacea can cause significant cosmetic defects and psychological damage to the patient. To avoid serious consequences from these problems, the treatment of rosacea should be multi-component with the involvement, if necessary, of different specialists (dermatologists, cosmetologists, nutritionists, endocrinologists, psychologists).
In the absence of timely treatment, the progression of rosacea leads to severe infectious skin lesions with the risk of generalization of the infection with corresponding complications. In addition, elements of severe rosacea can be injured, ulcerated, followed by bleeding.
Tactics
When the first signs of rosacea appear, as well as with the progression of already existing forms, the ineffectiveness of the previously prescribed treatment, a visit to a dermatologist is indicated.
The initial visit to a specialist is the most important, since it is necessary to carry out the entire range of diagnostic measures, followed by the appointment of individual treatment.
An immediate visit to a specialist is indicated if there has been a mechanical damage to the skin in the area of rosacea, as well as if any changes in appearance are noticed or previously absent sensations have appeared.
Rosacea is a chronic pathology that lasts for a long time, for many years, with periods of exacerbation and improvement. The course of the disease may depend on various factors occurring in a person’s life, therefore, close contact with a specialist should be maintained, with the help of whom a timely and adequate response to the ongoing changes in the skin will be carried out.
It is also important to realize the need for preventive consultations on the management of rosacea, especially before the upcoming changes in life: choosing a diet and diet, before changing the usual cosmetics, planning travel to zones with a different climate, changing a place of work with a different microclimate, as well as when starting another treatment affecting the human endocrine system.
Treatment
Treatment for rosacea is multicomponent and individual, and also depends on the severity of the symptoms. Conservative treatment includes:
- Drug therapy;
- Local cosmetic treatment;
- Correction and elimination of provoking factors;
- Treatmet of concomitant pathology;
- A therapy aimed at reducing emotional distress.
For the treatment of the erythematous form, it is enough to eliminate the etiological factors and the use of cosmetic products. When papular-pustular elements appear, local antibiotic therapy is prescribed. Systemic use of antibiotics is indicated for phimous rosacea.
Local treatment should include anti-inflammatory drugs, azelaic acid and other groups of drugs according to indications (for example, affecting the tone of the vascular wall of blood capillaries).
For the treatment of telangiectasias, methods of laser and electrocoagulation are used. Minor skin blemishes can be repaired with dermabrasion. Severe phimosis forms of rosacea are subject to surgical treatment in combination with conservative therapy and active prophylaxis.
It is important to understand that there is no single miracle remedy that can, in a short time, quickly, without consequences, and absolutely help every person in the fight against rosacea. That is why you need to be critical of the advertising of such drugs and self-medication by them. Any new drug should be discussed with a specialist.
Also, in the treatment of rosacea, a clear consistency in actions and adherence to the implementation of recommendations is needed. Self-deviation from the prescribed treatment regimen, interruption and non-compliance with therapeutic regimens significantly complicates the achievement of the expected effect.
At the same time, it is necessary to understand the risk of failure in treatment, to accept that the prescribed therapy does not always have the desired effectiveness and speed of achieving results. There should be a readiness for an open dialogue with a dermatologist, tolerance for a possible change in approaches to treatment.
Prevention
Prevention of rosacea consists in a gentle and careful attitude to the skin, timely treatment of infectious diseases, strengthening immunity, proper and high-quality personal hygiene, in maintaining a healthy lifestyle, especially in terms of nutrition.
To eliminate negative consequences and complications, it is necessary:
- Limiting ultraviolet exposure (tanning bed, sun tanning);
- Use of protective creams during periods of active sun;
- Exclusion of chronic skin trauma;
- Limitation or elimination of ionizing radiation, occupational hazards;
- Compliance with safety measures when working with factors damaging the skin;
- Personal hygiene and basic skin health awareness.
A regular examination of the skin, timely consultation with a dermatologist are also necessary if any changes appear on it.